Don't miss our updates



Ovarian rejuvenation with PRP (platelet-rich plasma) is an innovative technique that many fertility centers use to improve ovarian function in women with low ovarian reserve or premature ovarian insufficiency. These promising results can increase your chances of success in an IVF treatment. However, choosing the right timing for the application is key. Here we clarify when to do it, how it works, and in which cases it is most effective. What is ovarian rejuvenation with PRP and what is it for? It involves injecting platelet-rich plasma — extracted from your own blood — directly into the ovaries. Its growth factors stimulate cellular regeneration, improving follicular activity and oocyte quality. It is recommended in cases of: Low ovarian reserve. Premature ovarian insufficiency. Poor oocyte quality. Advanced maternal age in IVF. Repeated IVF failures. Do not self-medicate: consult a reproductive specialist before deciding on any treatment. When is the best time to perform ovarian rejuvenation with PRP during the IVF cycle? There are three key phases: 1. 2–3 months before ovarian stimulation Applying PRP with this lead time allows the growth factors to act on ovarian tissue to improve: Egg production. Oocyte quality and fertilization rates. Reduction of hormonal doses. 2. During ovarian stimulation If the ovarian response is poor, some specialists apply PRP mid-cycle to: Improve the response in real time. Increase the number of mature oocytes. Its effects may take time to manifest, so it is not always the ideal option. 3. After an embryo transfer failure For those who have suffered implantation failure, PRP can improve endometrial receptivity: Enhances endometrial quality. Reduces uterine inflammation. Aids in cases of recurrent implantation. How does ovarian rejuvenation with PRP work? Blood draw: 10–20 mL of venous blood. Processing: Centrifugation to isolate platelet-rich plasma. Ovarian injection: 2–4 mL of PRP in each ovary, guided by transvaginal ultrasound. Monitoring: Ultrasounds and hormonal tests to assess response. This outpatient procedure is minimally invasive and allows you to resume your activities in less than 24 hours. Who can benefit from ovarian rejuvenation with PRP? Low ovarian reserve (low AMH). Premature ovarian insufficiency (< 40 years). Women > 35 years with poor oocyte quality. Poor ovarian response in previous cycles. Recurrent implantation failure. Although it does not guarantee success, studies and data from specialized centers show benefits, especially if performed before stimulation. For complementary techniques, learn about IVF MORE®: an innovative technique for oocyte restoration. Final considerations Ovarian rejuvenation with PRP is a promising tool that, when properly indicated and at the right time, can make a difference on your journey to parenthood. Every case is unique: always consult a reproductive specialist to design the most suitable plan for you. Frequently Asked Questions 1. Is the PRP injection painful? It is performed under light sedation or local anesthesia. Discomfort is mild and transient, like cramps, and usually subsides within 24–48 hours. Relative rest and mild analgesics are recommended if needed. 2. How long does it take to see the effect? Growth factors begin to act immediately, but the most noticeable results appear at 2–3 months. That’s why it’s ideal to schedule it before ovarian stimulation. 3. Are there risks or side effects? Being autologous, the risk of allergies is virtually nil. There may be local inflammation, infection (rare), or mild pain. It is essential to perform it in a sterile environment with qualified personnel. 4. Can I combine PRP with other IVF treatments? Yes. PRP is usually used alongside standard stimulation protocols to enhance ovarian response and improve oocyte quality. Consult your specialist to design the best treatment plan. Sources Consulted American Society for Reproductive Medicine. (2020). Platelet-rich plasma and ovarian rejuvenation. Fertility and Sterility, 113(2), 207–217. MedlinePlus. (2021). Infertility treatments. U.S. National Library of Medicine. Lee, J. et al. (2019). Autologous platelet-rich plasma for ovarian rejuvenation in women with poor ovarian response. Journal of Assisted Reproduction and Genetics, 36(8), 1673–1685. National Institutes of Health. (2022). Premature ovarian insufficiency. NIH. We are with you every step of the way. If you have questions or need personalized guidance, turn to a reproductive assisted specialist: your desire to become a mother or father deserves the best care.
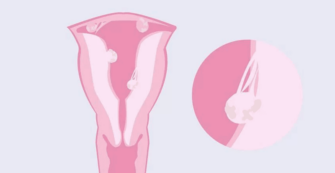
For many couples, becoming a mother or father is one of life’s most exciting and rewarding moments. But when fertility issues arise, that dream can feel increasingly distant. A common cause of infertility in women is pelvic adhesions, also called scar tissue. They develop after abdominal or pelvic surgeries, infections, endometriosis, or trauma in the area, and can hinder both conception and proper pregnancy development. In this article we explore what pelvic adhesions are and how they affect fertility. What are pelvic adhesions and why do they form? Pelvic adhesions are bands of scar tissue that bind organs—ovaries, tubes, uterus, bladder, and intestines—causing loss of mobility and normal function. They form when the body repairs inflammation or injury after surgery, infection, or endometriosis. Ovaries can become stuck to other structures, making egg release difficult. Blockage or distortion of the tubes prevents the egg and sperm from meeting. The risk of ectopic pregnancy increases if the tubes are compromised. Pain during intercourse can lead to avoiding it during fertile days. How do pelvic adhesions affect fertility and pregnancy? They interfere with gamete transport, tubal patency, and embryo migration. If the tubes are blocked or twisted, sperm cannot reach the egg, and the embryo cannot implant properly in the uterus. They also increase the risk of ectopic pregnancy (learn more about ectopic pregnancies). Assisted reproduction techniques, such as IVF, bypass these issues by retrieving eggs directly from the ovaries and transferring healthy embryos to the uterus. What symptoms may suggest the presence of adhesions? Chronic pelvic pain Very painful periods Pain during sex Difficulty conceiving Sometimes intestinal obstruction Higher risk of ectopic pregnancy Risk factors for pelvic adhesions C-section or ovarian cyst removal Myomectomy (fibroid removal) Endometriosis surgery (What is endometriosis and how does it affect fertility?) Appendicitis or pelvic inflammatory disease (from STIs like chlamydia) Infections such as hydrosalpinx Between 60% and 90% of women who undergo gynecological surgeries develop adhesions. Laparoscopy reduces the risk but does not eliminate it. Pelvic adhesions How are adhesions safely diagnosed? Laparoscopy is the gold-standard test but can create new adhesions. At Ingenes we prefer a non-invasive transvaginal ultrasound (TVUS) first and sometimes a hysterosalpingography (HSG) with contrast (10–20 mL), which only causes mild discomfort. Treatments to conceive with pelvic adhesions IVF is the most effective option since it bypasses the tubes. Eggs are retrieved from the ovaries, fertilized in the lab, and the highest-quality embryos are transferred to the uterus, increasing pregnancy chances. Do not self-medicate: always consult a fertility specialist to design a personalized plan that maximizes your chances. What to do if you suspect you have pelvic adhesions? See a reproductive endocrinologist for a comprehensive evaluation. With your medical history, imaging tests, and personalized advice, you can choose the most appropriate treatment. At Ingenes, we support you with empathy and professionalism every step of the way toward motherhood or fatherhood. Remember to always consult a specialist before making any decisions or starting any treatment. Frequently Asked Questions 1. Can pelvic physiotherapy prevent or treat adhesions? Specialized pelvic physiotherapy improves circulation and tissue mobility, relieving pain and stiffness, but does not eliminate fibrosis. It is usually combined with medical treatments under specialist supervision. 2. Is laparoscopy safe for treating adhesions if I want to get pregnant? Laparoscopy minimizes risk compared to open surgery, using 5–10 mm incisions. However, there is still a chance of forming new adhesions. Your doctor will weigh benefits and risks based on your history and reproductive goals. 3. How long should I wait after surgery before trying to conceive? It is recommended to wait between 3 and 6 months for tissues to regenerate and inflammation to subside, although the exact time depends on the type of surgery and your recovery. Always follow your specialist’s guidance. 4. What is the success rate of IVF in women with pelvic adhesions? It depends on factors such as age, egg quality, and severity of adhesions. Generally, women under 35 can achieve over a 50% chance of clinical pregnancy per cycle. A personalized assessment will provide more precise figures. References American Society for Reproductive Medicine. Adhesion Prevention and Management. Fertility and Sterility, 113(2), 443–455 (2020). MedlinePlus. Pelvic Adhesions. U.S. National Library of Medicine (2023). Chapron C., Souza C., Gonzalez F. Adhesion Formation After Endometriosis Surgery: A Multicenter Trial. Journal of Minimally Invasive Gynecology, 25(5), 805–812 (2018). Stratton P., MacLean A. Pelvic Adhesions: Impact on Fertility and Role of Laparoscopy. Human Reproduction Update, 25(4), 457–471 (2019).

Here you are going to learn what microbiota is and how it is related to your fertility and some advice to take of it, promoting better reproductive health. The human body has 10 times more bacteria or microbes than human cells. Among them, it is formed a group of genetic information that makes good health possible. Nevertheless, it is very important to keep a balance because the microbiota could be affected. What is microbiota? It is a group of microorganisms that allows us to live healthily. It is composed of a number of elements that are affected by the following factors: Which patients should check on their microbiota? The medical examination for the good health of the microbiota is not part of the group of routine checkups to verify well reproductive health. However, it is essential to do it for the next cases: Some possible causes It is possible that a condition or health issue leads to the inflammation of the microbiota and then the microbiota allows the entering of negative bacteria, resulting in the impossibility of the embryo to grow. Some of those conditions could be the following: Studies of microbiota in fertility cases have been directed just in women because it is about the relation between the endometrial and its bacterial composition with the possible implantation and the development of the embryo inside the uterus. Imbalance in the microbiota or dysbiosis symptoms To present any type of inflammation or imbalance in the microbiota could be asymptomatic. However, it is possible to present the next signs and symptoms: Diagnosis To make sure you have any imbalance in the microbiota or dysbiosis, it is recommended to perform a hysteroscopy-guided biopsy. Nevertheless, it is possible to perform a laboratory culture study. Don’t forget that… If you are a woman of reproductive age, don’t hesitate to consult Gynecology and Assisted Reproduction experts at a minor inconvenience. In the same way, don’t forget to have annual routine checkups to keep an eye on any situation Becoming a mother is possible in almost any case thanks to Assisted Reproductive Technologies and medical advances. An imbalance in the microbiota or dysbiosis will not stop your dream from coming true. Ingenes Fertility Institute in Mexico has a wide range of programs and treatments of high and low complexity to you to bring a baby home.

Low egg quality affects many women worldwide and can feel like an insurmountable obstacle to conception. Sadness, frustration, and despair are common reactions, but remember: you are not alone. Receiving this diagnosis does not mean you cannot have children. With the right treatment and a hopeful attitude, you have several paths to achieve your dream. Instead of letting it overwhelm you, take control and work with a team of specialists to choose the ideal plan. From in vitro fertilization to complementary therapies and lifestyle changes, there are alternatives that can help you become a mother. How do I know if my egg quality is low? Women are born with about 2 million oocytes, but by the start of puberty only around 400,000 remain. Each cycle only 350 to 450 mature, and their quality depends on biological and environmental factors. To confirm it, always consult a specialist in Assisted Reproduction. Meanwhile, review these 10 factors that influence egg quality. What causes poor egg quality? 1. Maternal age Ovarian reserve and egg quality decline with age, especially after 35. This change can surprise many women. 2. Overweight and obesity Excess weight affects multiple systems and reduces both the number and maturity of oocytes. Women with obesity often retrieve fewer mature eggs and face lower pregnancy rates. 3. Cancer treatments Chemotherapy and radiotherapy diminish ovarian reserve and egg quality. If facing a cancer diagnosis, consider oocyte vitrification before starting treatment. 4. Hormonal imbalances Conditions like Polycystic Ovary Syndrome prevent proper egg maturation and affect its quality. 5. Genetic factors Some mutations harden the egg’s zona pellucida, hindering fertilization and increasing the risk of abnormal divisions. 6. Ovarian stimulation The type of hormone, dose, and duration of stimulation in assisted reproduction cycles influence egg quality. 7. Endometriosis Endometrial tissue outside the uterus impairs ovarian function and egg quality, depending on the available reserve. 8. Alcohol consumption The WHO recommends a maximum of 0.5 glass of wine per day. During assisted reproduction treatments, it’s best to avoid alcohol 3 to 6 months beforehand. 9. Smoking Tobacco releases toxins that alter ovulatory hormones and accelerate menopause, reducing egg quality. 10. Immune problems Disorders like insulin resistance affect metabolism and oocyte cellular function. Proper management improves quality and success rates. Irai and Sofía, Ingenes family How can I improve my egg quality? Adopt a healthy lifestyle: balanced diet, regular exercise, and avoid self-medication. Before taking any supplement or medication, consult an Assisted Reproduction specialist. Explore studies like “What We Know About Oocyte Quality and Its Impact on Fertility” and “Infertility Factors: Understanding Ovarian Reserve” to better understand your options. Does poor egg quality prevent having a baby? No. With support from an expert team and a personalized plan, many women achieve a successful pregnancy. Read the testimony of Iraí, who overcame this diagnosis and now enjoys her daughter Sofía. If you have been trying for over a year or have been diagnosed with low egg quality, don’t give up. Your determination and specialist support are your greatest strengths. Frequently Asked Questions What are the symptoms of low egg quality? There are no obvious symptoms; it’s detected with hormonal tests (FSH, AMH) and ovarian reserve ultrasounds measuring antral follicles. FSH >10 mIU/mL or AMH 10–12), age, and medical history complete the diagnosis. Your specialist will propose the most suitable action plan. Can I improve my egg quality with supplements? Antioxidants like vitamin E, coenzyme Q10, and folic acid help reduce oxidative stress. Still, do not medicate without medical supervision. Each case is unique. Your specialist will review your tests and suggest supplements only as support to a healthy diet and lifestyle. Does stress affect egg quality? Chronic stress raises cortisol and other hormones that interfere with oocyte maturation. Practices like meditation, yoga, or therapy help reduce it. Including relaxation activities before and during IVF improves your well-being and treatment outcomes. When should I see a specialist? If you are over 35 and have not conceived after six months of trying, or if there is a history of endometriosis, chemotherapy, or other risk factors, consult an assisted reproduction expert. Early diagnosis offers more options: ovarian reserve tests, genetic evaluation, and personalized treatment plans. Sources Consulted American Society for Reproductive Medicine. (2020). Assessing ovarian reserve: Practice Committee document. Fertility and Sterility. doi:10.1016/j.fertnstert.2020.03.018 MedlinePlus. (2021). Oocyte quality. Retrieved from https://medlineplus.gov/ovarianreserve World Health Organization. (2019). Global status report on alcohol. Retrieved from https://www.who.int/publications/i/item/9789241565639 European Society of Human Reproduction and Embryology. (2022). Endometriosis and fertility. Human Reproduction. doi:10.1093/humrep/deac123 We are with you every step of the way. For an accurate diagnosis and a plan tailored to your situation, trust an assisted fertilization specialist. Your dream of building a family can come true.

Helen remembers the moment her life took an unexpected turn. At 33, after facing years of health challenges such as endometriosis, the loss of an ovary, and multiple operations for cysts, Helen’s life seemed to move further and further away from her dream of becoming a mother. “When you’re young, you don’t think about the future consequences of these health problems,” she shares. “But when I decided to start a family, reality hit me hard.” After years of unsuccessful treatments and visits to numerous gynecologists, Helen’s hope was fading. The emotional burden of not being able to conceive weighed on her, deeply affecting her well-being and her relationships. “Everything I saw reminded me of what I couldn’t have. I cried all the time, I felt like I had given up.” This struggle not only wore Helen down emotionally but also led to the collapse of her marriage. It was then that, amid desperation, Helen’s mother told her about Ingenes Fertility Institute in Mexico. “I will never forget that moment. It was when I realized that my problem was not unique and that there was hope.” At Ingenes, Helen was diagnosed with polycystic ovaries, a new twist in her already complex medical history. However, this time, she felt supported and understood. “The doctors were incredible. They didn’t just treat me; they connected with me on a very personal level.” The personalized support and treatment at Ingenes led Helen to a moment that would change her life forever: the discovery of her pregnancy. “It was like receiving the best gift imaginable. There was nothing that compared to the joy of knowing that she was going to be a mother.” But the surprise was even greater when Helen found out that she would not only have one baby, but two. “Hanna and Haén came into my life as a double miracle, choosing me as their mother.” This event not only gave Helen the family she had longed for but also allowed her to celebrate something very special: the unique connection that only siblings can share. On National Siblings Day, Helen reflects on the meaning of having twins and the joy Hanna and Haén bring to her life. “Seeing them together, experiencing life side by side, fills me with indescribable happiness. They are a constant reminder that, despite challenges, hope must never be lost.” Helen’s story is a testament to perseverance, faith, and the power of medical science that helps transform the dream of motherhood into a reality. At Ingenes Fertility Institute in Mexico, she found not only her solution to her fertility problems but also a community that accompanied her on her journey toward finding her baby. Today, Helen looks to the future with optimism, embracing every moment with Hanna and Haén. “They chose me, and I found the right path to reach them,” she says with a smile. “Now I know that miracles come twice.”

Losing weight, having a new car or house, and having a better-paying job are just some of the goals we set for ourselves each year. Some we achieve, and many others remain in the attempt. However, has having a baby been among your goals? How long have you wanted it without achieving it? The circumstances may be many, but it is time for that purpose not to remain just another unfulfilled wish. For this reason, we give you five resolutions so that you can decide this new year and improve the process of finding your baby at home since they will not only improve your health in general but will also promote your fertility. From purposes to realities 1.-Eat healthy Changing our eating habits is one of the goals that will bring the most benefits this year if you decide to do it since it will improve your weight and body composition. In this sense, start this process by avoiding processed or canned foods, choose and increasing your consumption of fruits and vegetables, making sure your preparations are lower in fat, and increasing your consumption of natural water. With these small changes, you will see the difference not only on the scale but in your mood as you prepare your body for that long-awaited path of being a mother. It is a purpose that complements the first, accompanying your new good eating habits with a daily exercise routine will not only keep you in shape but will accelerate and improve your chances of getting pregnant. Everything is better with professional help 3. Avoid bad habits Drinking alcohol in excess and smoking decreases the quality of eggs and sperm since their substances produce toxicity in the hormones involved in ovulation. In this same sense, it is important to mention that if you plan to have a baby, cutting down on caffeine will favor your goal, since it is scientifically proven that drinking more than three cups a day can make it difficult for the egg to implant in the uterus. If you have been trying to be a mother for more than a year and have not succeeded, it may be a fertility problem. This is verified through a series of personalized studies, where they diagnose the main problem that you or your partner may have, and based on this, they guide you to the best treatment that allows you to fulfill the dream of being a mother. Possibly you have already made several attempts and have not achieved that long-awaited goal, and it is evident that discouragement, stress, frustration, and sadness are the order of the day. It is completely understandable because you do not always understand the reasons why you have not been able to have a baby; However, all those negative emotions such as stress only hinder the process and negatively affect your chances of conceiving. Taking life calmly and minimizing stress as much as possible will make the process much better. Don’t let another year go by with an unfulfilled wish, and this 2024 let us help you lower your star from the sky. We guarantee that you will not be alone in this important process in your life. Go ahead and schedule an appointment, with Ingenes Fertility Institute in Mexico if it is possible!
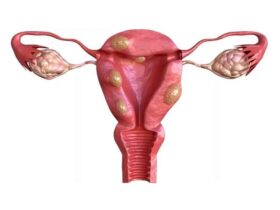
Uterine myomatosis is the formation of myomas or fibroids inside the uterus. These are benign tumors classified according to their location. Depending on where they are found, fibroids are classified as: Intramural: within the muscular wall of the uterus. They can affect fertility if they exceed 4 cm. Submucosal: on the surface of the uterine lining. They hinder embryo implantation. Subserosal: in the outer layer of the uterus. They usually do not interfere with fertility. What is uterine myomatosis and why does it matter for fertility? Uterine myomatosis involves the growth of fibroids, benign smooth muscle tumors, inside the uterus. It affects about 20% of women of reproductive age, especially after age 30. Fibroids can range from microscopic nodules to masses over 4 kg, altering the shape of the uterus and reducing pregnancy chances. How common is uterine myomatosis in those trying to conceive? Uterine fibroids are the most common pelvic tumors in women of reproductive age, present in nearly 70–80% before menopause. Although many are asymptomatic, those that deform the uterine cavity—particularly large intramural and submucosal fibroids—are involved in up to 80% of uterine factor infertility cases. How do fibroids affect embryo implantation? Large submucosal and intramural fibroids can: Alter sperm transport and uterine peristalsis Reduce endometrial receptivity by compressing the lining Increase the risk of implantation failure and early miscarriage Can fibroids complicate pregnancy? Yes. During pregnancy, fibroids can cause: Higher risk of miscarriage and preterm birth Fetal growth restriction due to lack of space Cervical canal obstruction or labor dystocia Postpartum hemorrhage from poor uterine contraction What symptoms may indicate fibroids? About 25% are asymptomatic. When symptoms occur, they include: Sensation of pelvic pressure or heaviness Heavy or prolonged menstrual bleeding Pelvic cramps and irregular bleeding Frequent urination or difficulty urinating Secondary infertility or recurrent miscarriages Severity depends on fibroid size, number, and location. How is diagnosis confirmed? Transvaginal ultrasound is the gold standard, with nearly 100% sensitivity (95% transabdominal). In complex cases, MRI is used. Always consult a reproductive medicine specialist to interpret results and design a treatment plan. Fertility-preserving treatment options Choice depends on age, fibroid characteristics, and reproductive goals: Expectant management for small, asymptomatic fibroids Myomectomy (surgical removal), followed by assisted reproduction techniques Controlled ovarian stimulation combined with in vitro fertilization (IVF) if cavity distortion persists IVF bypasses uterine transport obstacles and allows for selecting the embryo with the highest implantation potential. For more information, see our guide on Endometriosis: what it is and how it impacts fertility. FAQ 1. Can small fibroids disappear on their own? Yes. Many remain stable or shrink after menopause due to estrogen decline. In reproductive age, asymptomatic fibroids under 2 cm are usually monitored with periodic ultrasounds. If you plan to conceive, even a small submucosal fibroid can affect implantation, so consult your doctor to assess intervention before trying to conceive. 2. Are there non-surgical treatments? GnRH agonists and selective progesterone receptor modulators can temporarily shrink fibroids and reduce bleeding in 3–6 month cycles. They improve conditions before surgery or comfort but are not definitive solutions. Never self-medicate without medical supervision. 3. When can I attempt IVF after a myomectomy? Ideally between 6 and 12 months after surgery, before recurrence risk increases. This timing allows the uterine lining to heal and optimizes pregnancy chances. Make sure your specialist confirms proper healing with ultrasound or hysteroscopy before starting treatment. 4. Does the risk of miscarriage increase? Yes. Fibroids that deform the cavity or alter blood flow are associated with early pregnancy loss. Risk increases with fibroid size and location, especially submucosal and large intramural fibroids. Proper management, surgical or with assisted reproduction, significantly reduces miscarriage rates. Always consult a specialist before making decisions. References Faerstein, E., Szklo, M., & Schwingl, P. J. (2001). Risk factors for uterine leiomyoma: a practice-based case–control study. American Journal of Epidemiology, 153(5), 463–469. doi:10.1093/aje/153.5.463 Lau, W., & Shlisselberg, S. (2016). Management of uterine fibroids. American Family Physician, 94(2), 106–113. https://www.aafp.org/afp/2016/0715/p106.html MedlinePlus. (2021). Uterine fibroids. https://medlineplus.gov/uterinefibroids.html Stewart, E. A. (2015). Uterine fibroids. Lancet, 376(9745), 145–157. doi:10.1016/S0140-6736(10)60246-1 Remember: every body is unique. Stay informed, keep hope, and consult an assisted reproduction specialist for personalized care.
In the realm of family and career planning, egg freezing is an increasingly valued option for those who wish to postpone parenthood without giving up the possibility of having children in the future. At Ingenes, we offer this cutting-edge procedure so you can approach the timing of starting your family with confidence. What is egg freezing and what is it for? Egg freezing, or oocyte cryopreservation, allows you to store your eggs at –196 °C via vitrification, ensuring they maintain their quality and reproductive potential when you decide to use them. Who are ideal candidates for egg freezing? Women who want to focus on their careers or personal projects before becoming mothers. Those who prefer to wait to find the right partner. Anyone undergoing medical treatments (such as chemotherapy) that could affect fertility. Women concerned about the natural decline in egg quality with age. What is the process at Ingenes? Ovarian stimulation: Personalized hormones (150–300 IU daily) to develop multiple follicles. Follicular monitoring: Ultrasounds and blood tests to determine the ideal retrieval time. Egg retrieval: Outpatient procedure with light anesthesia to collect mature oocytes. Vitrification: Rapid cooling and secure storage in liquid nitrogen. Benefits of vitrifying your eggs Control over your motherhood timeline. Preservation of egg quality against aging. Peace of mind when facing fertility-threatening treatments. Time to find the ideal partner without biological pressure. Emotional support throughout the journey At Ingenes, we combine cutting-edge technology with a personal approach. Our fertility psychologists provide personalized counseling and support sessions so you feel accompanied every step of the way. Technology that maximizes oocyte survival State-of-the-art equipment: High-precision vitrification to minimize cellular damage. Innovative protocols: Over 90% of eggs survive thawing. Continuous monitoring: High-resolution ultrasounds and constant serum measurements. For more details visit Egg vitrification: an option to preserve fertility or discover if freezing eggs at 40 is viable. Frequently asked questions 1. At what age is it most effective? The success rate is higher before age 35, when ovarian reserve and egg quality are optimal. Always consult a specialist and avoid self-medication. 2. How long do frozen eggs last? They can be stored indefinitely at –196 °C. At Ingenes, we periodically review samples to ensure viability. 3. What is the success probability? It depends on age and egg count. At Ingenes, we report >60% oocyte survival and a 45% pregnancy rate in women under 35. 4. Does retrieval hurt? It is performed under light sedation or intravenous anesthesia, so you won’t feel pain during the procedure. Discomfort lasts 24–48 hours, and our team provides the best post-operative care. Sources consulted American Society for Reproductive Medicine. (2020). Practice Committee Opinion: Mature oocyte cryopreservation. Fertility and Sterility, 114(1), 108–115. https://doi.org/10.1016/j.fertnstert.2020.03.012 National Cancer Institute. (2022). Cancer Terms: Egg Freezing. https://www.cancer.gov/publications/dictionaries/cancer-terms/def/egg-freezing MedlinePlus. (2021). Egg freezing. https://medlineplus.gov/eggsfreezing.html Practice Committee ASRM. (2013). Mature oocyte cryopreservation: A guideline. Fertility and Sterility, 99(1), 37–43. https://doi.org/10.1016/j.fertnstert.2012.09.025 We’re with you every step of the way. Don’t hesitate to seek guidance from a fertility specialist to make the best decision for your motherhood journey.
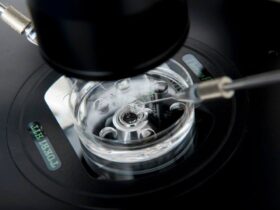
In Vitro Fertilization (IVF) and Intracytoplasmic Sperm Injection (ICSI) are advanced assisted reproduction techniques that have opened up a world of possibilities for many couples facing fertility challenges. At Ingenes, these techniques are fundamental pillars to help our patients achieve their dream of having a baby. What is IVF? IVF is a process in which eggs are removed from a woman’s body and fertilized with sperm in a laboratory. This procedure is ideal for overcoming various fertility problems, such as blockages in the fallopian tubes or complications with sperm quality. At Ingenes, we personalize each IVF treatment to maximize the chances of success. ICSI and its Importance ICSI is a specialized variant of IVF. It is mainly used in cases of severe male infertility, such as low mobility or number of sperm. In this process, a single sperm is injected directly into the egg. At Ingenes, ICSI has become a hope for many couples struggling to conceive. The IVF and ICSI Process at Ingenes The process begins with ovarian stimulation, followed by egg collection and fertilization in the laboratory. The resulting embryos are observed and the best quality ones are selected for transfer to the uterus. At Ingenes, this process is carried out with the highest technology and the care of fertility experts. Why Choose Ingenes for Your IVF or ICSI Treatment? Choosing the right center for IVF or ICSI treatment is crucial. At Ingenes, we not only have cutting-edge technology and a highly qualified team, but we also offer a comprehensive and personalized approach. Each patient receives a treatment plan tailored to their specific needs. Success and Support at Ingenes IVF and ICSI treatments have high success rates, especially at Ingenes, where we combine clinical experience with a human approach. Additionally, we provide emotional support throughout the process, understanding that fertility is both a physical and emotional journey. Overcoming Challenges with IVF and ICSI At Ingenes, we are committed to overcoming fertility challenges. Whether you are dealing with male or female infertility issues, our IVF and ICSI techniques are designed to give you the best chance of having a baby. Your Journey Toward the search for your baby We know that the journey towards finding your baby can be complicated, but with Ingenes, you are not alone. Our goal is to make the process as clear and comfortable as possible, giving you the confidence and support you need. Ready to take the next step in your journey towards the arrival of your baby? At Ingenes we are here to guide you every step of the way. Contact us today to learn more about our IVF and ICSI treatments and how we can help you fulfill your dream of having your baby at home.

Becoming a mother is a decision filled with emotion and meaning. Lluvia decided to do it on her own at 40, embarking on a journey of courage and hope. Nowadays, more women choose to become mothers without a partner, either by conviction or life circumstances. Through Lluvia’s story you’ll learn about her motivations, the challenges she faced, and her experience as a single mother thanks to assisted reproduction. Discover how science opened doors for her and read real testimonials like “I Became a Mother at 40” and “I Wanted to Be a Single Mother and Finally Had My Babies at 46.” What motivates a woman to become a single mother at 40? Lluvia always felt a very strong maternal instinct. Upon turning 40, concerns about her biological clock and social expectations led her to decide: use her own eggs and a trusted friend as sperm donor. Avoid self-medication and seek professional guidance to assess your ovarian reserve with tests like AMH and antral follicle count. Before starting, consult a specialist in Assisted Reproduction to design a personalized plan. What challenges does single motherhood with IVF at 40 entail? Age reduces egg quality and quantity. After detecting a fibroid, Lluvia underwent myomectomy and waited eight months before IVF. She faced emotional stress, uncertainty, and the routine of daily FSH and LH injections (around 225 IU). Physical recovery and anxiety over success rates (below 30% for women over 40) test one’s strength. Having a team of a reproductive specialist, psychologist, and nutritionist makes a difference in outcomes and well-being. How to prepare for fertility treatments at 40 as a single woman? A diet rich in folates and antioxidants, 50 g of protein daily, avoiding tobacco and excess caffeine, and taking 400 µg of folic acid are good first steps. Moderate exercise, yoga, and mindfulness help hormonal balance. Have ovarian reserve tests, pelvic ultrasound, and infection screening done as soon as possible. Support from counselors or online groups reduces loneliness and maintains motivation. What support exists for single mothers undergoing IVF? Specialized clinics offer financial counseling, legal support for donation agreements, and psychological assistance. Online communities connect women with similar experiences, reducing isolation. Scholarship programs or shared risk plans lower costs, and the testimony of other mothers—like “I Became a Mother at 40”—provides practical advice and hope. Emotional journey after IVF success After a positive pregnancy test, many maintain cautious optimism. Lluvia waited until week 12 to share the news with her family. Celebrating each milestone—the first ultrasound, the heartbeat—reinforces confidence. Postpartum support is vital. Professional guidance and mother groups help with subsequent changes and ensure that mother and child thrive during the first year and beyond. Advantages of assisted reproduction for single mothers IVF, egg vitrification, and sperm donation expand the options for starting a family. Personalized protocols optimize chances, showing it’s no longer necessary to rely solely on adoption or co-parenting. Stories like Lluvia’s, Tony’s at 43, and Alba’s at 48 demonstrate that science and personal determination can challenge age limits and social conventions. FAQ on becoming a single mother at 40 1. What is the success rate of IVF for women over 40? Between 15% and 30% per cycle using own eggs, depending on ovarian reserve, embryo quality, and clinical experience. To improve outcomes, get AMH and AFC tests, optimize your lifestyle, and follow a personalized hormonal protocol. 2. Is it safe to use a sperm donor? Yes, if you choose a certified bank with genetic and health screenings. Legal and psychological counseling will help you manage ethical and emotional aspects. 3. How to manage emotional support during treatment? Cognitive-behavioral therapy, online groups, and support from family and friends are key. Relaxation, meditation, and mindfulness techniques reduce anxiety. 4. What costs does IVF involve and is financing available? A cycle can cost between $3,000 and $15,000 USD, plus $1,000–$5,000 USD in medications. There are payment plans, medical loans, shared risk programs, and some scholarships. Sources Consulted American Society for Reproductive Medicine. (2022). Assisted Reproductive Technology Success Rates. National Library of Medicine. (2023). Age and Fertility: What You Need to Know. MedlinePlus. European Society of Human Reproduction and Embryology. (2021). ESHRE Guidelines: Ovarian Stimulation. Centers for Disease Control and Prevention. (2020). CDC Fertility Clinic Success Rates Report. We are with you every step of this journey. If you are considering motherhood through assisted reproduction, consult a specialist to receive the best guidance and support.

What is an ectopic pregnancy and why does it happen? An ectopic pregnancy occurs when the embryo implants outside the uterus, almost always in the fallopian tubes, although it can also happen in the ovaries or the cervix. This occurs when something prevents the fertilized egg from reaching the uterus to grow as it should. Illustration of an ectopic pregnancy After experiencing an ectopic pregnancy, the most common question is: Can I get pregnant again? The good news is yes: around 40% of women achieve a subsequent pregnancy if the causes are properly identified and treated and with the guidance of an Assisted Reproduction specialist. How does a normal pregnancy occur, and what goes wrong in an ectopic? In a typical pregnancy: Ovaries: release a mature egg. Fallopian tubes: where the egg meets the sperm and fertilization occurs. Uterus: the ideal place for the embryo to implant and grow. If the tubes have adhesions, scars from infections (like chlamydia or gonorrhea), or prior surgery (for example, tubal ligation), the embryo cannot reach the uterus and implants elsewhere, causing an ectopic pregnancy. What are the symptoms of an ectopic pregnancy? From the start you may notice: Severe, constant pain in the lower abdomen, usually on one side. Light vaginal bleeding or brown spotting for several days. Nausea and dizziness, very similar to morning sickness. If the tube ruptures, you may experience: Intense, widespread abdominal pain. Rapid and weak pulse, cold and sweaty skin. Difficulty breathing or feeling faint. If you experience any of these symptoms, do not self-medicate and seek emergency medical attention. Who is at higher risk for an ectopic pregnancy? Common risk factors include: History of infections (chlamydia, gonorrhea). Endometriosis or pelvic adhesions. Tubal surgeries, including ligation or having only one tube. Smoking. Age 35 to 44 years. Congenital abnormalities in the fallopian tubes. How can I have a baby after an ectopic pregnancy? In vitro fertilization (IVF) is the safest route after an ectopic pregnancy because the egg and sperm unite in the laboratory, bypassing the tubes. The process includes: Ovarian stimulation with medication to obtain multiple eggs. Selection of the healthiest eggs and sperm. In vitro fertilization and embryo culture. Transfer of the highest-quality embryos to the uterus. Monitoring of hCG levels and embryonic development. Before making any decisions, consult an Assisted Reproduction specialist. They can design a tailored plan and increase your chances. At Ingenes we have an expert team in IVF and ectopic pregnancies to support you every step of the way. Frequently Asked Questions 1. Does the Risk of Another Ectopic Pregnancy Increase If I’ve Had One? The recurrence risk is 10–20%, depending on the health and function of your tubes. That’s why, before trying again, it’s advisable to perform an ultrasound and HSG to assess the tubes. If they’re damaged, IVF is the best option. 2. Can I Get Pregnant with Only One Tube? Yes. You retain a 50% chance of natural pregnancy thanks to the remaining ovary and tube. To improve success, IVF bypasses the tubes entirely. 3. Does IVF Hurt and What Are Its Risks? Egg retrieval is done under sedation, so there is no pain. Afterwards, you may experience mild discomfort and abdominal bloating. Risks are low: ovarian hyperstimulation (

What is egg freezing and what is it for? Egg freezing is an assisted reproduction technique that helps you pause your biological clock. Your mature oocytes are retrieved and vitrified in liquid nitrogen at –196 °C, where they can be stored for up to 27 years. Avoid self-medicating without consulting a doctor, as each ovarian stimulation protocol is adjusted to your age, ovarian reserve, and health status. How to know if egg freezing is right for you? If you want to postpone motherhood without losing options, this technique is your ally. The first step is to see a specialist in Assisted Reproduction. With an anti-Müllerian hormone (AMH) test and an antral follicle count (AFC) via ultrasound, you’ll assess your ovarian reserve and confirm if it’s the ideal time. What medical reasons drive egg freezing? Besides personal reasons, there are medical situations that make this decision advisable: Chemotherapy or radiotherapy that damages ovarian reserve. Gender transition. Autoimmune diseases or gynecological oncology surgeries. In these cases, vitrifying your oocytes opens a door of hope for your family plans. Do you need a partner to freeze your eggs? No. Unlike embryos, only your oocytes are stored here. If in the future you decide to fertilize them and don’t have a partner, you can use certified donor sperm from a sperm bank. Egg freezing process step by step Ovarian stimulation with hormones (FSH and LH) in personalized doses (e.g., 150–300 IU/day). Ultrasound monitoring and estradiol (E2) measurement in pg/mL. Retrieval of mature oocytes via follicular puncture under sedation. Vitrification of each oocyte with cryoprotectant to prevent ice crystals. Storage in liquid nitrogen tanks (<–196 °C). With Ingenes, your oocytes are protected by a unique chain-of-custody system. Alternatives and next steps In addition to egg freezing, you can consider: Embryo vitrification. Ovarian tissue preservation. We recommend reading “Egg freezing: a strategic decision for your family’s future” to learn how these options fit your life plan. At Ingenes we provide guidance at every stage: freezing eggs means gaining time with warmth and security. Frequently Asked Questions (FAQ) 1. Does egg freezing guarantee a future pregnancy? Success rates vary based on your age at vitrification and oocyte quality. Women under 35 have over 90 % survival after thawing and 50–60 % pregnancy rates per cycle. However, factors like embryo implantation and endometrial receptivity also play a role. That’s why it’s essential to see an Assisted Reproduction specialist. 2. What risks does ovarian stimulation carry? The main risk is ovarian hyperstimulation syndrome (OHSS), with abdominal pain, bloating and, in severe cases, pleural effusion or ascites (< 2 % with modern protocols). Other effects include breast tenderness, mood changes, and mild discomfort during retrieval. At Ingenes we monitor you closely to ensure your well-being. 3. How long can eggs be stored? Vitrification keeps them viable for decades. There are cases of pregnancies after 27 years of storage. Legally, the limit depends on the country: in Mexico it’s up to 10 years, renewable with your consent. 4. Can I change my motherhood plans? Yes. You can use your oocytes with partner or donor sperm in IVF cycles whenever you choose. Also, if the law allows, you can transfer embryos to a gestational carrier. At Ingenes we support you with legal and psychological counseling every step of the way. Sources Consulted Practice Committee of the American Society for Reproductive Medicine. (2020). Mature oocyte cryopreservation: a guideline. Fertility and Sterility, 114(4), 767–781. https://doi.org/10.1016/j.fertnstert.2020.06.025 American College of Obstetricians and Gynecologists. (2018). Committee Opinion No. 745: Patient education and informed consent. Obstetrics & Gynecology, 131, e196–e205. https://doi.org/10.1097/AOG.0000000000002586 MedlinePlus. (2023). Egg freezing. Retrieved from https://medlineplus.gov/eggsfreezing.html European Society of Human Reproduction and Embryology. (2022). ESHRE Guideline: Oocyte preservation. Human Reproduction Open, 2022(1), hoac004. https://doi.org/10.1093/hropen/hoac004 We accompany you on your journey to motherhood and fatherhood. Don’t hesitate to seek the support of a fertility specialist to answer your questions and design a personalized plan. We’re with you!

When you try to conceive a baby, the journey can be challenging and full of emotional and physical ups and downs. If you suffer from adenomyosis or another infertility condition, you know that doubts and fear can grow. Eridani’s story shows that there is hope. She overcame adversity thanks to Assisted Reproduction Methods and today enjoys the joy of being a mom. Eridani, proud Ingenes mom What is adenomyosis and how does it affect fertility? Adenomyosis occurs when the tissue that normally lines the uterus grows into its muscular wall. This often causes heavy bleeding (up to 200 ml per cycle), pelvic pain, and an enlarged uterus (sometimes 1–2 kg heavier). All of this can make embryo implantation difficult and reduce natural fertility. Some women have severe cramps, others mild discomfort. It is usually diagnosed between ages 40 and 50, but it also affects women in their 30s and even late 20s. It is detected with a transvaginal ultrasound or MRI. Treatments range from hormonal therapy to minimally invasive surgery, always tailored to your motherhood goals. Do not self-medicate: always consult a specialist. How did Eridani overcome adenomyosis to conceive? “I told Enrique, ‘If you want, find someone else, I’m the problem.’ It was very hard. My life was just work until I got married and discovered my longing to become a mom.” After almost 3 years of trying in Mexico and New York with no results, she came to Ingenes. There they confirmed endometriosis, adenomyosis, and poor egg quality. With a personalized ovarian stimulation protocol (225 IU of FSH daily) and careful embryo culture, she achieved a successful twin pregnancy. Ingenes babies feeding Assisted reproduction options for adenomyosis It depends on your age, the severity of adenomyosis, and your motherhood plans. Options include: Hormonal suppression (GnRH agonists) to reduce the uterus by up to 30% in 3–6 months. Minimally invasive surgery (adenomyomectomy) to remove lesions and preserve the uterus. In vitro fertilization (IVF) with stimulation and frozen embryo transfer. Before any medication or procedure, consult a specialist in Assisted Reproduction. Emotional and practical tips during treatment Keeping stress under control and a healthy lifestyle helps a lot. Try: Yoga or mindfulness to reduce cortisol. A diet rich in omega-3 and antioxidants. Support groups or therapy to share experiences. With your partner’s love and your trusted network, the process will be more bearable. Proud Ingenes parents with their daughters For more inspiring testimonials, visit: I became a mom despite having endometriosis and I had uterine fibroids and became a mother with IVF. How to start your journey to motherhood with adenomyosis? Schedule an evaluation with a fertility specialist. They will review your history, perform imaging studies, and propose a personalized plan. Early detection and timely treatment can make all the difference. Frequently Asked Questions 1. Can adenomyosis go away on its own? No. Without intervention it usually worsens, with more bleeding and pain. Early diagnosis allows for medical management that improves your quality of life. 2. Does it affect pregnancy outcomes? It increases the risks of miscarriage, preterm birth, and placental complications. With personalized protocols, such as GnRH pre-treatment before IVF, success rates improve. 3. Natural remedies for pain? Thermotherapy, anti-inflammatory diets, and supplements (omega-3, turmeric) can help, but never replace medical treatment. Always consult your doctor. 4. Adenomyosis vs. endometriosis? Both involve endometrial tissue outside its normal location. In endometriosis it is on pelvic organs and the peritoneum; in adenomyosis, it is within the uterine muscle. Management differs, so good imaging is key. Sources consulted American College of Obstetricians and Gynecologists. Practice Bulletin No. 228: Management of Endometriosis. Obstetrics & Gynecology, 135(4), e65–e81. doi:10.1097/AOG.0000000000003774 National Library of Medicine. (2021). Adenomyosis. MedlinePlus. https://medlineplus.gov/adenomyosis.html Harmsen, M. J. A., et al. (2019). Adenomyosis: Prevalence, risk factors and therapeutic options. Best Practice & Research Clinical Obstetrics & Gynaecology, 65, 40–49. doi:10.1016/j.bpobgyn.2019.01.002 Vercellini, P., et al. (2017). Medical treatment for adenomyosis: A systematic review. International Journal of Obstetrics & Gynaecology, 124(1), 3–8. doi:10.1111/1471-0528.14301 We are with you every step of the way. Remember that seeking professional help in assisted reproduction could be the key to making your dream of becoming a mother or father come true.

In in vitro fertilization (IVF), science and hope unite for those dreaming of welcoming a baby. We explain the process from start to finish. How is in vitro fertilization performed step by step? 1. Ovarian stimulation: you receive hormones (150–300 IU of FSH/LH) so your ovaries develop multiple follicles. 2. Follicular puncture: under light sedation, mature eggs are retrieved with an ultrasound-guided needle. 3. Semen preparation: we collect a 2–5 mL sample and select the most motile sperm. 4. In vitro fertilization: oocytes and sperm are placed together in a ~100 µL culture medium. After 16–18 h the zygote forms, and at 48 h it becomes a 4–8 cell embryo ready for transfer. When is IVF recommended? Damage or blockage of the fallopian tubes. Moderate to severe endometriosis. Severe male factor (low count or motility). Women ≥35 years with reduced ovarian reserve. Failures in other fertility treatments. Before starting, consult an assisted reproduction specialist; they will tell you if this treatment is the best path for you. Preparation for your IVF cycle Your doctor will request hormonal tests (FSH, LH, AMH), a transvaginal ultrasound, and a semen analysis. Adopt a healthy lifestyle: balanced diet, moderate exercise, and stress management. Avoid tobacco and alcohol at least 3 months beforehand. You can also seek nutritional counseling and psychological support to feel accompanied at every stage. Follicular puncture and fertilization The puncture takes 20–30 minutes with local anesthesia or sedation. An average of 8–15 eggs are retrieved. In the lab, we assess quality and fertilize them by conventional IVF or ICSI, depending on your case. Embryos grow in incubators at 37 °C, 5 % CO₂, and 95 % humidity until reaching the blastocyst stage (day 5). Embryo transfer and beyond Between day 3 and 5, we select 1–2 top-quality embryos and deposit them in your uterus under ultrasound guidance. The procedure is brief; afterward you’ll rest for 24–48 h and receive progesterone (600 mg/day vaginally or 50 mg IM). Two weeks later, a serum beta-hCG test is performed. If positive, you continue hormonal support until weeks 10–12 of gestation. For a deeper dive into each phase, visit Understand in vitro fertilization step by step and Understand in vitro fertilization. Frequently asked questions 1. What influences success rates? Maternal age (<35 years up to 40% success vs. 20% at 40), egg and sperm quality, and lab experience. Lifestyle habits, body mass index, and infertility causes also matter. 2. Does it hurt or carry risks? The main discomfort is the follicular puncture, managed with sedation. Hormonal injections may cause mild discomfort. Risks: ovarian hyperstimulation (1–5%), mild bleeding or infection, and multiple pregnancy if multiple embryos are transferred. 3. Can I use donors? Yes, if your ovarian reserve or sperm quality is low. Donors undergo genetic, infectious, and psychological screening. The IVF protocol is the same; only the gametes change. 4. When will I know if I’m pregnant? You wait 10–14 days post-transfer for the beta-hCG test. If positive, a heartbeat is confirmed by ultrasound at 5–6 weeks and obstetric follow-up begins. Sources American Society for Reproductive Medicine. Practice Committee Guidelines. Fertility and Sterility (2021). MedlinePlus. In Vitro Fertilization. U.S. National Library of Medicine (2022). European Society of Human Reproduction and Embryology. Vienna Consensus on GnRH analogue protocols in ART (2020). National Institute for Health and Care Excellence. Fertility: Assessment and treatment (2017). Remember: each path to parenthood is unique. If you have questions or want more information, consult an assisted reproduction specialist. You are not alone on this journey!

Pregnancy is one of the most exciting and meaningful stages in a woman’s life. However, for mothers who have experienced a high-risk pregnancy, the path to motherhood can be overwhelming and full of uncertainties. This is where Maternal-Fetal Medicine comes in. From medical complications to emotional fears and insecurities, mothers in these situations need all the support and attention they can get. Over the last few decades, Maternal-Fetal Medicine has been a branch of medicine comprised of a team of professionals dedicated to providing the best possible care for mothers and babies in high-risk situations. With their dedication, expertise, and passion for what they do, these doctors and specialists have helped thousands of women overcome the challenges presented by these pregnancies. This is the story of Marlene, who at 13 weeks into her twin pregnancy, faced complications but tackled adversity with the support of specialists. “Both in my family and my husband’s family, there were histories of infertility” I was at a point in my career where I wanted to change jobs and pursue a Master’s degree. We had many plans, but my husband first suggested the idea of starting a family. Both in my family and my husband’s family, there were histories of infertility. We weren’t in a rush to get pregnant, but we were worried that we might also face infertility issues like our families had. When you decide to become a mother, you realize the commitment and sacrifice that it entails. You discover a love that you never knew before, one that is different from the love you have for your husband or parents; it’s something beautiful and new. “They told me it was difficult for my babies to make it” I remember going to my gynecologist, and she told me everything was fine. I didn’t take long to get pregnant with twins, and everything was going smoothly until I had that bleeding at 13 weeks. The procedure recommended to me is normal when there’s a risk of miscarriage, but in my case, it was too early in my pregnancy, and they told me it would be difficult for my babies to make it. I decided to seek a second opinion, and that’s how I ended up at the institute – in a wheelchair, with heavy bleeding, and no hope. Despite the fear, I found unique human warmth and was given a lot of confidence. If I hadn’t come here, my children probably wouldn’t have been born. “In the Maternal-Fetal Medicine Unit, they supported me to continue my pregnancy” I was able to conceive naturally, and we had the idea that the institute was only a fertility clinic, but I found out that it goes beyond that. In the Maternal-Fetal Medicine Unit, they supported me to continue my pregnancy without any setbacks and ensure my twins were born healthy and strong. Now, in addition to my children, I am 17 weeks pregnant. Here, I have the envelope that indicates the sex of my baby, but I will wait to open it with my family. I am very excited, I don’t know if there will be blue balloons or pink balloons, although everyone is expecting it to be a girl. I celebrate becoming a mother again, a role that completely changed my life. Your children become the center of your universe and the most beautiful commitment. It is there when you discover that new love, and you simply feel that your life is complete.” View this post on Instagram A post shared by Ingenes Institute (@ingenesinstitute) The Maternal-Fetal Medicine Unit is here for you The process of becoming a mother is long and goes through different stages that are usually not easy. However, with the company of your loved ones and highly trained specialists, everything can be possible for you to enjoy every moment to the fullest. If you, like Marlene, have encountered obstacles during your pregnancy, do not hesitate to approach Ingenes. Share your story with us by clicking here!

The term Ubuntu may not be familiar to many, but its essence surrounds us, connects us and, at Ingenes, we embrace it in our daily lives. Originally from the Bantu languages of Africa, Ubuntu translates as “humanity towards others”, but its meaning goes much further. In the awareness that our actions affect those around us, and how, through connection and community, we can positively influence the lives of others. What is Ubuntu? Ubuntu is an ancient African philosophy that focuses on the interconnectedness of all. It is an idea that reminds us that we are all part of a great community and that our existence is linked to that of others. The word comes from the Bantu language and is understood as a traditional African concept that emphasizes the importance of community, cooperation, and interconnectedness. Ubuntu in everyday life More than a word, Ubuntu is a way of living. It refers to empathy, to understand that our actions have repercussions in the world and in the people around us. It is the awareness that we depend on each other, in our personal relationships, at work, and also in the environment. Ingenes and the philosophy of Ubuntu At Ingenes, Ubuntu resonates in every corner. Our commitment to the community and the importance of caring for each other is a reflection of this philosophy. Every time we provide support, advice, or a solution to those who dream of starting a family, we do so with the understanding that we are part of an interconnected network. Thus, by helping people build a family, we are contributing not only to their happiness but also to the strength and well-being of the community as a whole. Ubuntu can be summed up in a simple but powerful phrase: “I am because we are”. At Ingenes, we recognize and value this interconnectedness, and we are proud to work every day so that more people achieve the dream of having their baby at home.

The National Family Day is an opportunity to pause and recognize the richness of every family story in the United States. Today, families take many forms: from traditional to the most diverse, reflecting the openness and change of our society. What is National Family Day and why celebrate diversity? National Family Day is the day to honor every type of family: nuclear, single-parent, same-sex and more. It’s about celebrating inclusion, equality, and the unconditional love that binds every family, regardless of its structure. How has the American family evolved? According to Pew Research Center (2022), the nuclear family remains present, but other models have grown: Single-parent: rose from 12% in 1968 to 27% in 2014. Same-sex: over 1,000,000 same-sex couples living together in 2020 (Statista, 2021). Single parents by adoption or assisted reproduction, with IVF and egg donation. Single-parent families: challenges and strengths The increase is due to divorces, planned motherhood and assisted reproduction. Challenges include: Greater economic and time burden on a single caregiver. Need for support networks and attention to mental health. But these families also demonstrate great resilience and deep love. Impact of same-sex parenting With marriage equality and legal recognition, over 1,000,000 same-sex couples have formed families, contributing: Parenting based on empathy and conscious communication. Greater visibility and inclusion in public policies. Support on your path to parenthood At Ingenes we offer IVF, ICSI, egg and sperm donation with personalized protocols. Before self-medicating, consult a specialist in Assisted Reproduction to receive the guidance and follow-up your family deserves. We take every step with you, with empathy and expertise, because your dream of becoming a parent is unique and valuable. Celebrate family diversity all year round Events, resources and awareness campaigns keep family inclusion alive. For more ideas and actions, visit our article Celebrating family pride and diversity in June. Frequently Asked Questions (FAQ) What is assisted reproduction and how does it help different families? Techniques like IVF and ICSI assist couples with infertility, single mothers and same-sex couples, ensuring high-quality embryos. Always consult a medical specialist and avoid self-medication. What are the emotional challenges of a single-parent family? The responsibility of a single parent can generate stress and anxiety. Having support networks, help groups and therapy strengthens the emotional health of the whole family. How to promote inclusion of same-sex families at school? Equality policies, workshops and diverse materials raise awareness among educational staff. The participation of mothers and fathers in committees and collaboration with LGBTQ+ associations ensure safe environments. What resources support the mental health of first-time parents? The American Psychological Association and local groups offer guides and hotlines. A psychologist or family therapist can prevent burnout and strengthen the new dynamic. Sources Consulted Pew Research Center. (2022). Family Structures in America. Statista. (2021). Number of same‐sex couples in the United States. MedlinePlus. (2023). In Vitro Fertilization. American Society for Reproductive Medicine. (2022). Definition of infertility. Fertility and Sterility, 118(6), 1431–1442. Remember: every family is unique and every path to parenthood deserves professional attention. If you’re ready to take the next step, see a specialist in assisted fertilization and start your journey with the best support.

Assisted Reproduction is a complex and emotional issue that affects many couples worldwide. As Assisted Reproduction techniques continue to evolve, so do the questions and concerns of people seeking options to start or expand their family. In this article, we will address some of the most frequently asked questions about Assisted Reproduction, from what in vitro fertilization is to how long the entire process can take. If you are considering Assisted Reproduction as an option for yourself or those around you, it is important that you are fully informed and prepared to make important and well-founded decisions. Keep reading to learn more about Assisted Reproduction and how you can achieve your dream of becoming a mother. These are the most frequently asked questions about Assisted Reproduction: How can I know when my menstrual cycle starts? An average menstrual cycle lasts for 28 days, and it is counted from the first day of bleeding. If you have been taking contraceptives, your cycle will start between 5 and 7 days after stopping them. Do I have to come on the second day of my period for the transfer test? No, the transfer test can be done at any time during the cycle as long as the patient is not menstruating. I am taking medication for ovarian stimulation, and I am feeling very swollen, is this normal? The ovarian stimulation treatment causes the ovaries to increase in size, which can generate a feeling of heaviness in the abdominal area and a little inflammation. These symptoms can also occur after egg retrieval. I am on treatment with patches, and they promised to call me, but they haven’t, what should I do? The patches contain estradiol, which is used to prepare the endometrium to receive the embryo, so they are used in treatments such as egg donation or frozen embryo transfer. Typically, patients attend a check-up eight days after starting treatment with patches. If more than 20 days have passed, and you have not received any calls, you should contact your treating doctor to receive instructions on the treatment to follow. Today is my last day of using patches, do I stop using them, or do I have to continue? It is not yet time for my embryo transfer. If it is not yet time for your embryo transfer, you should not stop using the patches for any reason. Their use should be continued until the treating doctor indicates otherwise, and once the time comes, they should be gradually stopped. My egg retrieval was today, when is my transfer? In most cases, embryo transfer is performed on the third day of embryo culture. However, there are some occasions where it may be beneficial to opt for extended embryo culture (in which embryos are transferred up to the fifth day of development) to facilitate the selection of those with higher quality and greater implantation potential. This decision is made based on each patient’s history and the level of embryonic development. If my pregnancy test was positive, when do I need to make an appointment? If your pregnancy test was positive, your first check-up should take place after two weeks to define the location of your pregnancy through an ultrasound. If you experience severe pain or heavy bleeding before this appointment, it is important to contact your treating physician for instructions. Is this my first gestational ultrasound? Do I need to drink water? If your pregnancy test was positive, your first check-up should take place after two weeks to define the location of your pregnancy through an ultrasound. If you experience severe pain or heavy bleeding before this appointment, it is important to contact your treating physician for instructions. I’m pregnant and I have a headache, can I take something? It is recommended that you check your blood pressure before taking any medication, especially if you are more than 20 weeks pregnant. If your blood pressure is normal, you can take pain relievers such as paracetamol. Otherwise, it is important to contact your doctor, as headaches can be a symptom of conditions such as preeclampsia. I have a cold and my throat hurts a lot, what can I take? If you have a cold and are pregnant or undergoing ovarian stimulation treatment, it is recommended that you rest, drink plenty of fluids, and contact your treating physician to indicate an analgesic. Paracetamol does not affect either of these cases. I’m pregnant and I have cramps and bleeding, what should I do? If you are in the early weeks of pregnancy, it is important to rest and contact your treating physician to indicate what you should do. You can also apply Indocid suppositories to prevent complications. If the bleeding is very heavy or if you are more than 12 weeks pregnant, it is important to contact your doctor immediately, who should perform an ultrasound to ensure everything is fine. Is a gynecological screening or fetal risk test necessary? The gynecological screening should be performed in all patients without exception, as it allows the presence of genetic abnormalities in the fetus to be ruled out. Thanks to being performed by ultrasound, this test does not carry any risk. When should I have the gynecological screening or fetal risk test? Do I have to fast? This should be carried out between the 11th and 13th week of pregnancy and does not require fasting. I had a semen analysis and they were supposed to call me but they haven’t. What should I do? If you had a semen analysis and have not received your results, either by phone or in person, you should contact your treating doctor to deliver them to you and explain what they mean. What is the address of the institute and how can I get there? Visit our Ingenes branches How much does an assisted reproduction treatment cost? Reproductive and fertility treatments are very complex procedures that require the cooperation of a team of experts in various disciplines such as Embryology, Biology, Andrology, and Psychotherapy, among
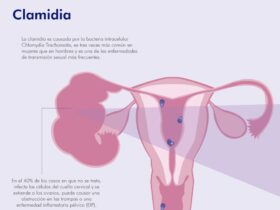
On the journey to motherhood or fatherhood, every step matters. Every hope, every dream, and every challenge brings us closer to the moment when our desire to conceive becomes reality. But sometimes unexpected obstacles arise, such as chlamydia, a silent infection that can affect our fertility. It is essential to understand how chlamydia can interfere with our plans and how we can face it with courage. Chlamydia, often surrounded by stigma and shame, can make conception difficult. However, let’s focus on our strengths and take charge of our sexual and reproductive health. Below we will see how we can protect ourselves, diagnose, and treat this infection to pave the way toward our longed-for goal: starting a family. What is chlamydia and how does it affect fertility? Chlamydia is one of the most common sexually transmitted infections (STIs) and often goes unnoticed. Caused by the intracellular bacterium Chlamydia trachomatis, it is three times more frequent in women than in men. According to the Centers for Disease Control and Prevention (CDC), around 2.8 million cases are reported each year in the U.S. In 40% of untreated cases, the infection rises from the cervical canal to the ovaries, fallopian tubes, or uterus, causing pelvic inflammatory disease (PID) or tubal blockage. It can impede fertility in several ways: Cervical infection: hinders sperm passage. Ovarian infection: alters ovulation, reduces ovarian reserve, or forms abscesses. Fallopian tube infection: causes hydrosalpinx (fluid accumulation) and increases the risk of ectopic pregnancy. Endometritis: inflames the endometrium and hinders embryo implantation. Inflammatory adhesions: obstruct the transport of oocytes and sperm. Pain during intercourse: may lead to avoiding sex on the days of highest fertility. During pregnancy, untreated chlamydia can cause: Ectopic pregnancy Spontaneous abortion Amniotic fluid infection Premature membrane rupture Preterm birth Low birth weight Neonatal pneumonia or conjunctivitis Main symptoms of chlamydia Chlamydia is often “silent”: up to 75% of infected women show no symptoms. When they appear (1–3 weeks after exposure), they may include: Abnormal vaginal discharge Burning or discomfort when urinating Bleeding between periods Pain during intercourse (dyspareunia) Pelvic pain or fever Infertility If you notice any of these signs, avoid intercourse and see a doctor as soon as possible. Early diagnosis prevents PID and greater damage to your fertility. How is chlamydia diagnosed? Diagnosis includes reviewing medical history, a brief pelvic exam, and collecting a cervical or vaginal sample for nucleic acid amplification testing (NAAT). Urine or blood tests can also detect antibodies. The CDC recommends annual chlamydia screening for sexually active individuals under 25 and for older women with risk factors. Pregnant women should be tested routinely. Since chlamydia and gonorrhea often coexist, it is advisable to test for both. In advanced cases, a transvaginal ultrasound may be necessary to assess pelvic damage. If I test positive and want to conceive, what should I do? If you test positive, abstain from intercourse until you and your partner(s) complete treatment and receive negative follow-up tests. Reinfection is common if only one person is treated. If there is tubal damage, in vitro fertilization (IVF) is the best option, as it bypasses damaged tubes. It is vital to treat the infection before starting an IVF cycle to improve success rates. Do not self-medicate; before taking any drugs, consult a reproductive specialist for proper guidance. Treatment options First-line treatment is azithromycin 1 g in a single dose or doxycycline 100 mg every 12 h for 7 days. Sexual partners must be treated simultaneously to avoid reinfection. Follow-up testing at 3 months is recommended to confirm eradication. If PID has developed, hospitalization and intravenous antibiotics may be necessary. After treatment, a fertility evaluation will guide next steps. How to prevent future infections Always use condoms, limit the number of partners, get regular tests, and maintain open communication with your partner. Routine gynecological visits help detect and treat infections early. Related resources More information at Positive Chlamydia: Symptoms, Causes and Diagnosis. Frequently asked questions 1. Can chlamydia clear up on its own? Some mild cases may resolve without treatment, but relying on this is risky. Without antibiotics, the infection can ascend, cause PID, damage the tubes, and increase the risk of infertility and transmission to your partner or baby. Treatment is the only safe way to eradicate it. 2. How long should I wait after treatment before trying to conceive? After completing medication, wait at least 7 days before resuming sexual activity. A test of cure is recommended at 3 months or sooner if symptoms recur. For IVF, confirm eradication before the cycle; your specialist will advise based on your reproductive health. 3. Does chlamydia affect ovarian reserve? Inflammation from chlamydia can reduce ovarian reserve or disrupt ovulation. While the direct link needs more study, you can assess your reserve with antimüllerian hormone (AMH) testing and antral follicle count via ultrasound. Speak to your reproductive endocrinologist if you have a history of chlamydia. 4. Is it safe to undergo IVF after a chlamydia infection? Yes, IVF is safe and recommended if there is tubal damage. Treating the infection beforehand protects the uterus and improves implantation. Your specialist may perform imaging studies and possibly give antibiotics around the transfer to minimize risks. References Centers for Disease Control and Prevention. (2023). Sexually Transmitted Disease Surveillance. https://www.cdc.gov/std/statistics/2023/default.htm Workowski, K. A., & Bolan, G. A. (2015). Sexually Transmitted Diseases Treatment Guidelines, 2015. Clinical Infectious Diseases, 61(8), e1–e42. https://doi.org/10.1093/cid/civ784 MedlinePlus. (2023). Chlamydia. https://medlineplus.gov/chlamydia.html World Health Organization. (2016). Global health sector strategy on sexually transmitted infections 2016–2021. https://www.who.int/reproductivehealth/publications/rtis/ghss-stis/en/ We are with you on this journey: having children is a deep and achievable desire. Do not hesitate to seek help from a fertilization specialist for the support and guidance you deserve.

What are uterine fibroids and how can they impact fertility? Uterine fibroids are noncancerous growths in the muscle layer of the uterus. They can be as small as a pea or grow several centimeters wide, appearing inside the cavity, within the wall, or on the outer surface. Many women notice no symptoms, but some experience heavy periods, pelvic pressure, or discomfort. When fibroids change the shape of the uterine cavity or affect blood flow to the lining, they can make it harder for an embryo to implant and raise the chance of miscarriage. Why did it take me 10 years to conceive despite multiple treatments? “My husband and I married young—I was almost 20—and decided to wait before starting a family. When we tried to get pregnant naturally, nothing happened. An ultrasound showed ovarian cysts, so I started contraceptive pills as part of the treatment plan, and we scheduled our first insemination that November.” “I was 23 and hoped for success, but after six inseminations, we still had no baby. Every appointment ended in tears. I kept asking the doctors what was wrong, but I never got clear answers.” How did IVF with fibroids lead to success on the first transfer? Daniela, Ingenes mother, and her family “In 2016 we tried IVF at another clinic with two embryos, but it didn’t work. In 2019, we found this institute. They saw small fibroids on the outside of my uterus and reassured me they wouldn’t interfere. In September they transferred one embryo—and on the first try, it stuck. I cried tears of joy when the doctor called to say I was pregnant. After almost ten years of waiting, it finally happened.” What was my pregnancy and birth experience like after fibroids? Daniela and Angelina, Ingenes family “My pregnancy went smoothly. On May 17, 2020, my water broke early in the morning and by 7 a.m., our daughter Angelina was born. It was so fast! When they placed her in my arms, I felt like I was dreaming—tiny fingers, tiny toes. My husband was by my side, talking and kissing my belly all through pregnancy. That pure love carried us through every moment.” “All those years of frustration melted away the moment we met her. She completed our family.” What should you know before starting fertility treatment with fibroids? Never self-medicate. If you’re thinking about fertility treatments, talk to a reproductive specialist first. Fibroid size, position, and type vary greatly, and only a personalized assessment can determine the best plan for you. To read more success stories, visit “I had uterine fibroids and became a mother with IVF” or “I have endometriosis and got pregnant after 10 years”. FAQ 1. Can small fibroids outside the uterus really not affect IVF success? Yes. Subserosal fibroids—those on the outer uterine wall—usually don’t change the shape of the cavity or interfere with implantation if they’re under 3 cm and asymptomatic. Specialists use ultrasound or MRI to check size and location. Always discuss your individual case to decide if surgery is needed or if you can go straight to IVF. 2. What are common treatments for fibroids when trying to conceive? Treatment depends on fibroid type, size, symptoms, and your fertility goals. Medical options include short-term GnRH agonists or antagonists to shrink fibroids, with possible side effects like hot flashes. Surgically, myomectomy can be done by hysteroscopy (for inside-cavity fibroids), laparoscopy (small outer fibroids), or open surgery (large or multiple fibroids). Recovery before trying pregnancy ranges from 1 to 6 months, depending on the approach. 3. How does the IVF protocol change for women with fibroids? Ovarian stimulation is similar—gonadotropins to grow around 10–20 follicles with estradiol (E2) monitors in pg/mL. The main adaptation is ensuring the transfer catheter navigates any contour changes in the uterus, often using ultrasound guidance. Many women with small, non-distorting fibroids proceed with a standard protocol and achieve great results. 4. What follow-up care is recommended after giving birth post-IVF with fibroids? After delivery, track your menstrual cycle and fibroid growth with regular exams and pelvic ultrasounds every 6–12 months. If heavy bleeding (>80 mL per cycle) or pain returns, discuss medical or surgical options. Maintaining a healthy weight (BMI 18.5–24.9), a fiber-rich diet, regular exercise, and supplements like vitamin D and omega-3s may help slow fibroid growth. References American College of Obstetricians and Gynecologists. (2021). Uterine Fibroids. https://www.acog.org MedlinePlus. (2022). Uterine Fibroids. https://medlineplus.gov/uterinefibroids.html Pritts, E. A., Parker, W. H., & Olive, D. (2020). Fibroids and infertility: an update. Obstet Gynecol, 135(4), 28S–34S. doi:10.1097/AOG.0000000000003722 Somigliana, E., Vercellini, P., Parazzini, F., et al. (2019). Fibroids and ART outcomes: systematic review. Hum Reprod Update, 25(1), 130–142. doi:10.1093/humupd/dmy035 Stay hopeful: every journey is unique. If you’re facing fibroids and fertility challenges, reach out to a specialist in assisted reproduction. You don’t have to go through this alone.

Low ovarian reserve and a positive IVF result on her third attempt: this is Claudia’s story, who became mother to little Guillermo after visiting several fertility clinics and overcoming multiple failed assisted reproduction attempts. Claudia shares her challenges, the prejudices and misinformation she faced when deciding to have a baby after age 35, how she reached 37 weeks of pregnancy with a healthy baby, and how she dealt with a COVID-19 diagnosis shortly after her positive beta. What is low ovarian reserve and why does it affect my IVF? Low ovarian reserve means you have fewer follicles and quality eggs. After age 35, egg quantity and quality naturally decline. This reduces the success rate of a first IVF cycle to around 50–60%. Do not self-medicate; always consult an Assisted Reproduction specialist before making decisions. How does a multicycle treatment help women with low ovarian reserve? The multicycle program offers up to 3 IVF cycles with a refund guarantee if pregnancy is not achieved. Before transfer, the body is prepared with medications and hormones, respecting dosages in mL and application times. Although the first two attempts may not succeed, each cycle provides valuable information to adjust ovarian stimulation. What are the chances of success on the third IVF attempt? After two unsuccessful cycles it’s normal to feel discouraged. However, on the third attempt the chances increase if the medical team adjusts the gonadotropin dose and optimizes embryo quality. This story of persistence shows that combining medical adjustments and emotional support can lead to the desired outcome. How to manage complications like COVID-19 during pregnancy? A COVID-19 diagnosis after transfer can be frightening. Follow-up with prenatal checks every 2–4 weeks and laboratory tests (PCR, complete blood count) helps ensure the infection doesn’t affect pregnancy progression. Always consult your Assisted Reproduction specialist before taking any medication. I have low ovarian reserve and want a baby, what are my options? There are alternatives like egg donation, initial assessment programs, and high-complexity treatments. At Ingenes we offer the Initial Program and a team of highly experienced specialists. This story shows that each process is unique and deserves a plan tailored to you. Sources consulted Practice Committee of the American Society for Reproductive Medicine. (2020). Age and fertility: a committee opinion. Fertility and Sterility, 114(4), 850-857. doi:10.1016/j.fertnstert.2020.04.010 American College of Obstetricians and Gynecologists. (2018). FAQ: Fertility testing. Obstetrics & Gynecology, 131(1), e1-e4. doi:10.1097/AOG.0000000000002450 Gleicher, N., Kim, A., & Barad, D. H. (2017). Female age and ovarian reserve testing: A guide for clinicians. MedlinePlus. Retrieved from https://medlineplus.gov/ency/article/007198.htm De Vos, M., Smitz, J., & Woodruff, T. K. (2018). Fertility preservation in women: Practical guidelines. Human Reproduction Update, 24(6), 569-591. doi:10.1093/humupd/dmy025 Frequently asked questions 1. Does low ovarian reserve always prevent pregnancy? Not necessarily. Although there are fewer follicles, IVF with personalized stimulation allows retrieval of available eggs and obtaining quality embryos. Emotional support and good nutrition also make a difference. The key is a complete ovarian reserve assessment (AMH, AFC) and an individualized plan. Many patients with low reserve achieve pregnancy after 2 or 3 IVF cycles. 2. What risks are associated with undergoing multiple IVF cycles? Risks include mild ovarian hyperstimulation, emotional stress, and hormone side effects (abdominal pain, mood changes). With ultrasound monitoring and estradiol measurement in pg/mL, the team adjusts doses to prevent complications. The multicycle program with refund eases financial and emotional burden by offering peace of mind if pregnancy isn’t achieved after several attempts. 3. How do age and stress affect fertility? After age 35, egg quality and quantity decline and aneuploidies increase. Stress can disrupt the hypothalamic-pituitary-ovarian axis and affect ovulation. Relaxation techniques and psychological support improve ovarian response and implantation rates. 4. Why choose an assisted reproduction specialist? A specialist has training in reproductive medicine, hormonal management, minimally invasive surgery, and embryology. Their expertise ensures accurate diagnosis and a treatment adapted to your case. With over 20 years of experience and thousands of patients, Ingenes is a benchmark in Latin America for its results and humanized care. We know this journey is challenging and we want to support you every step of the way. If you’re considering starting treatment or have questions, don’t hesitate to seek the guidance of a fertility specialist. You are not alone in this process!
At Ingenes San Diego we understand how important this journey is for you. Our team combines cutting-edge technology with a close, personal approach to accompany you at every step, from the first evaluation to the most advanced reproductive techniques, always adapting to your needs. Who we are and what we offer We are a leading fertility clinic in assisted reproduction (ART). Here we perform in vitro fertilization (IVF), intracytoplasmic sperm injection (ICSI) and preimplantation genetic testing (PGT) in ISO-certified laboratories. We also offer egg vitrification, semen analysis and embryo culture with the highest quality standards. Our services: Comprehensive fertility evaluations (hormone panels, ultrasound) IVF/ICSI cycles with up to 1.5 mL of medium per embryo PGT for aneuploidy detection Egg and sperm cryopreservation Egg and sperm donation programs Counseling and emotional support throughout your process Your IVF process step by step 1. Ovarian stimulation and monitoring We personalize your protocol with daily injections (150–300 IU of follicle-stimulating hormone). We perform ultrasounds and estradiol measurements to track your follicle growth and choose the ideal time for egg retrieval. 2. Egg retrieval and fertilization Under light sedation, we use a 17-gauge needle to aspirate follicles in ≤10 mL of flushing medium. Eggs undergo IVF or ICSI depending on semen quality. 3. Embryo culture and transfer Embryos grow for 5–6 days in incubators with time-lapse imaging. We transfer one high-quality embryo to the uterus using a soft, ultrasound-guided catheter. Surplus embryos are vitrified at –196 °C. Why choose us? Our clinical pregnancy rates reach up to 55% per cycle in women under 35. We offer personalized counseling, financial plans and 24/7 support. Our certified reproductive endocrinologists design each protocol to maximize your safety and results, avoiding self-medication. We have geneticists, embryologists and mental health specialists to support you in every aspect of your path to parenthood. If you’re looking for nearby options, visit Ingenes Mexicali or discover Ingenes Fertility Specialists for home-based care. Key advantages Advanced genetic screening to reduce miscarriage risks Low-stress embryo transfers Comprehensive support: nutrition, psychology and finances CAP and CLIA accredited laboratory Frequently asked questions 1. How do I know if I need fertility treatment? If you’ve tried to conceive for more than 12 months (or 6 months if you’re over 35), consult a specialist. Irregular cycles, recurrent losses or conditions like PCOS and low ovarian reserve are signals to evaluate your fertility with hormone tests, ultrasounds and semen analysis. 2. What risks does IVF have and how do you manage them? IVF can cause ovarian hyperstimulation syndrome (OHSS), multiple pregnancies or procedural complications. At Ingenes we adjust doses, use “freeze-all” when necessary and transfer a single embryo to reduce risks. We have facilities and equipment ready for any eventuality. 3. Can I come if I live outside the U.S.? Yes. We assist with travel, visas and accommodation. We offer telemedicine and coordinate a comfortable stay in San Diego. If you prefer closer to Mexico, visit our sister clinic Ingenes Mexicali, with cultural and language support. 4. What emotional support do you offer? We have therapists specialized in reproductive health, support groups and individual sessions. We also offer mindfulness workshops and nutritional counseling so you don’t face this process alone. Sources American Society for Reproductive Medicine. Guidelines on Ovarian Stimulation. 2022. National Library of Medicine. In Vitro Fertilization. MedlinePlus. 2021. ESHRE Special Interest Group. Good Practice Recommendations for IVF Laboratories. Human Reproduction Open, 2020. Practice Committee ASRM. Criteria for Number of Embryos to Transfer. Fertility and Sterility, 2021. We’re with you every step of the way on this adventure. Don’t hesitate to seek accompaniment from an assisted reproduction specialist to resolve your doubts and care for your health.
Turner Syndrome is a condition caused by the partial or complete absence of the X chromosome, and it mainly affects women. Most people have 46 chromosomes in each cell (23 from the mother and 23 from the father). This syndrome develops on the 45th chromosome and occurs when a woman has one normal X chromosome while the other X chromosome is missing, incomplete, or has some alteration. How can Turner syndrome be present? The symptoms that appear in different stages and vary depending on the physical and growth characteristics of the person who has it, may include the following: Before birth During birth or childhood During teenage and adulthood Significant accumulation of fluid in the back of the neck or other abnormal fluid accumulations Cardiac abnormalities Abnormal kidneys Wide or webbed neck Low-set ears Broad chest with widely spaced nipples High and narrow palate Arms that turn outward at the elbows Narrow and upward-turned fingernails of both hands and feet Swelling of the hands and feet Slightly shorter height than average Delayed growth Heart defects Low hairline at the back of the head Small or receding lower jaw Short fingers and toes Ovarian insufficiency Growth delay Lack of expected onset of sexual changes during puberty Sexual development that stops during the teenage years Early cessation of menstrual cycles that is not due to pregnancy Infertility Turner Syndrome can affect the proper development of various systems in the body of the person who has it, but it varies according to each case. The complications can be: How to Detect Turner Syndrome? In conclusion, Turner Syndrome is a genetic disorder that can impact women’s lives in many ways. Early detection of this syndrome is crucial in order to take preventive measures and provide appropriate treatment. The PGT-A test is a useful tool that can help detect Turner Syndrome in embryos prior to transfer. This preimplantation genetic testing can identify chromosomal abnormalities in the embryo and ensure that only normal embryos are selected for transfer. Detecting Turner Syndrome through PGT-A testing can provide couples with greater peace of mind and confidence in the IVF process, as it increases the chances of a successful pregnancy and a healthy baby. At Ingenes Fertility Institute in Mexico, we offer a variety of preimplantation genetic testing services, including PGT-A, that can help detect Turner Syndrome and other chromosomal abnormalities. Our team of experts is committed to providing personalized, high-quality care to help couples achieve their reproductive goals. If you or someone you know is interested in detecting Turner Syndrome, do not hesitate to contact us for more information about our services.

Fertility issues affect 1 in 8 couples worldwide, of which 60% hide their reproductive problem from their surroundings and only 5% seek psychological help to cope with it. It has been identified that between 25% and 65% of couples experience stress when receiving a diagnosis of infertility. Research has shown that women receiving treatment for infertility have a level of “stress” similar to women dealing with life-threatening diseases such as cancer and heart disease. Infertile couples experience chronic stress every month, first with the hope of conceiving and then dealing with the disappointment of not having succeeded. How does stress work? Stress is a behavioral discomfort that arises from environmental tensions that an individual perceives as threatening, pressuring, or frustrating. In general terms, stress is defined as the feeling of self-doubt about being capable of facing certain situations over a determined period of time. In the case of infertility, individuals generate a series of personal, couple, and social pressures and ideas after failing to fulfill their dream of having a baby. People who are experiencing stress overload may exhibit some of the following symptoms: The desire to have a baby can be so strong that it often becomes the sole focus of our attention. As a result, if something in the search process is not done in a timely manner, the concern about not knowing what is happening can lead to significant stress. I want to have a baby, what’s next? It’s important to keep in mind that fertility testing and assisted reproductive treatments can be physically, emotionally, and financially stressful. That’s why it’s ideal to seek out specialists in Assisted Reproduction and receive comprehensive care. This is to ensure that you feel supported and confident in the decisions being made during this process. I’m having fertility problems and don’t know where to turn We understand the toll that fertility problems and reproductive processes can take. That’s why we approach patient care from both medical and emotional aspects to maximize the chances of success. Specifically, to provide a complete service to our patients, we have the Ingenes Emotional Support made up of a group of experts who specialize in addressing emotions related to fertility problems. Through this comprehensive support, we aim to help our patients improve their emotional well-being and ultimately increase the success of their treatment. Don’t hesitate to share your story with us!
Nowadays, even though there is an increased open mind to reproductive health issues because of the scientific progress in that matter and easier access to information, Assisted Reproduction keeps being a social taboo. It is a pointed-out topic, criticized and accepted just by a percentage of people. In a society where every kind of scenario and experience exists, where cultures merge and preferences converge, where we discuss equality and seek equity, there still exists a stigma and doubt towards the highly studied methods to create life. Even if these methods help people to accomplish their dream of having a family. Prejudice doesn’t stop science and society, However, no matter if prejudice and ignorance are around reproductive health topics, there are a lot of examples of the world and its habitants going through major changes; it is the case of how family structures transformed. Now we have diverse families with different members not adjusted to the traditional mom, dad, and children composition. New family models At the time, there are a lot of types of families, such as: All of us have the right to have a family and it is proclaimed in the Universal Declaration of Human Rights. Thanks to research and constant Assisted Reproduction specialists’ investigation, almost everyone who wishes to have a baby, can make their dream come true: single mothers, heterosexual couples, and even people with tubal ligation or vasectomy. Assisted Reproduction: an opportunity for everyone Through assisted reproduction, we have found solutions for all kinds of people. The treatments are divided into two groups: Among all, IVF is the most popular because it has the highest success rates. It has changed the lives of people that would like to experience parenthood and for any reason have not achieved it. Not just for physiological reasons, but also for those who have been delaying maternity and can’t avoid the famous “biological clock”. “Getting pregnant in a natural way and becoming moms and dads is science as well as it is through Assisted Reproductive Technology.” Says Dr. Martín Rivera, Medical Director of Ingenes Institute Guadalajara. Dr. Martín Rivera, gynecologist and biologist, shares his opinion on what involves assisted reproduction treatments and how this alternative has changed people’s lives despite the prejudices: “It is easy to doubt what is not familiar for us, even to keep a defensive posture, still if we are not well informed. Usually, we are afraid of accepting that there are a lot of options to accomplish something. Maybe because at one point society taught us that there is a specific and natural order of life. Nevertheless, everything has multiple ways to achieve what we are looking for. How many things don’t we wish to be following in order? Everything would be easier. Luckily, for what is not easy, scientific progress has given us solutions.” He adds: “Having a baby through treatment, requires a whole process, mental and physical. Because you need willingness, discipline, and a lot of love to make a sacrifice that people describe as something priceless.” How does assisted reproductive technology help people? Technology amazes a lot of people, confuses some, and worries others. What is innegable is that it never keeps adding results in favor of people that have all the love and conviction to become parents. However, being to get pregnant and having a baby are not the only benefits that assisted reproductive technology has achieved, it also allows us to: These make possible that more and more people understand the importance of reproductive medicine and specifically, assisted reproduction as an essential key to exercise the right to have a family. What do we do in Ingenes? In Ingenes, all our programs are focused to transform people’s lives with the arrival of a baby boy or girl. We help people who are fighting against fertility issues, and also those who decided to postpone their family life plans for the perfect time. We help single mothers, women couples, and whoever has the will to do all in their hands to have a child. From Artificial Insemination to In Vitro Fertilization, we use the highest technology in reproductive healthcare for women to achieve the result they are looking for, considering the less physical, emotional, and financial wear. Maybe some people still ask society to make a decision, and maybe some people don’t dare to mention it, but the results are there, the progress keeps going and every time there are more people accepting other options and approaching specialists. “Above all, the critics, and what others can say, Assisted Reproductive Technology changes lives and makes dreams come true”, Dr. Rivera declares.

Menopause is a time in a woman’s life when many experience significant physical and emotional changes. For some, it marks the end of their fertile stage, while for others, it may be the beginning of a new path toward motherhood. Although pregnancy during menopause may seem uncommon or impossible, many women have defied the odds and successfully conceived and carried a healthy baby to term. These women are true inspirations, demonstrating that there are no limits in life and that love and the desire to be a mother can overcome any obstacle. Pregnancy during menopause can also be an opportunity to reflect on life and the role of motherhood. It can be a time to find the inner strength necessary to face challenges and embrace the beauty and joy of creating life. However, it’s also essential to consider the potential risks and challenges that may arise during pregnancy in menopause, including complications such as preterm labor or preeclampsia. Therefore, it’s crucial to seek appropriate medical advice and receive the necessary emotional support to face these challenges. Pregnancy in menopause is a unique and exciting experience that can teach us about the power of love and determination. It’s a reminder that it’s never too late to pursue our dreams and create the life we desire. Keep reading for more details on pregnancy during the menopausal stage. Menopause nowadays Population change and growth have accelerated in recent decades throughout Latin America. The proportion of people over 60 years old has increased significantly; within this group, the majority are women. As a result of this phenomenon, there has been a formation of an adult population, resulting in a change in roles and social needs. What happens during menopause? In adult women, menopause signifies the end of menstruation and corresponds to a physiological event in a woman’s life that involves the termination of her reproductive cycle. With the onset of menopause, a woman’s menstrual period ceases due to the absence of hormones produced by the ovaries. While some women may not experience any other symptoms, as menopause approaches, it’s possible that the symptoms may include: During the stage called menopause or climacteric, there is a cessation of ovulation, meaning a woman’s reproductive life comes to an end, which limits conception. Can I be a mother during menopause? Fortunately, if a woman is in menopause and desires to have a baby, there are different alternatives. The most recommended option for these cases is egg donation, where young and healthy women provide eggs to women with depleted ovarian reserves, enabling them to carry a completely healthy pregnancy to term. This service is available at Ingenes for women up to 52 years old through an egg donation program, in which donor selection and evaluation are carried out according to parameters established by the American Society for Reproductive Medicine (ASRM). In this way, a woman can be assured that the procedures and reliability of the donation will comply with international safety and quality standards, achieving her goal of having a baby at home. Your dream can be possible! Learn more about Lorena’s story, who achieved her dream of becoming a mom through egg donation. We also have the story of Maria del Carmen, who at the age of 50 had the joy of bringing her little stars down to earth. Do not hesitate to share your story with us to find the best solution for you.
To understand how hypothyroidism influences fertility, first you need to know that the thyroid gland produces two key metabolic hormones: T4 (thyroxine) and T3 (triiodothyronine). This butterfly-shaped gland is located at the front of the neck, just below the Adam’s apple. Although there are many thyroid conditions, in this article we will focus on hypothyroidism and its impact on female fertility. Thyroid gland in the human body What is hypothyroidism and how does it affect fertility? Hypothyroidism occurs when the thyroid does not produce enough T3 and T4. In women it can disrupt ovulation, cause irregular menstrual cycles, and complicate conception. Do not self-medicate: before taking any medication, consult a Reproductive Medicine specialist. They will evaluate your case and increase your chances of pregnancy. Key symptoms in women trying to conceive Extreme fatigue Unexplained weight gain Cold intolerance Dry skin and brittle hair Irregular or absent menstrual cycles Mild depression or persistent constipation If you notice any of these changes, share them with your doctor. Recurrent miscarriages or difficulty conceiving can be warning signs. Most common causes of hypothyroidism Autoimmune thyroiditis (Hashimoto’s) Radiation therapy to the head or neck Thyroid surgery Iodine deficiency Medications (lithium, amiodarone) Pituitary disorders affecting TSH In many cases the cause is not identified, so early diagnosis is vital. Diagnosis before trying to conceive The endocrinologist will measure your neck, skin, weight, and heart rate. Then they will order a blood test to measure TSH. A value above 3.5 mU/L suggests hypothyroidism. Free T3 and T4 may also be measured to assess severity. With this data, your doctor will design a treatment plan to protect your health and that of your future baby. Treatment options if you plan to have a baby The standard treatment is levothyroxine, adjusted according to your weight (approx. 1.6 μg/kg per day) and lab results. Every body is unique: consult a Reproductive Medicine specialist to determine your dose and monitor your hormone levels. For more information, check our article Hypothyroidism and Fertility or explore Hyperthyroidism and Fertility. Ingenes family who overcame thyroid issues Frequently asked questions 1. Does hypothyroidism cause irreversible infertility? With treatment and TSH control, most patients regain ovarian function and can conceive naturally or with assisted reproduction techniques. 2. How do TSH levels influence embryonic development? TSH regulates T3 and T4, essential for ovarian follicle maturation and a receptive endometrium. Keeping TSH between 0.5–3.5 mU/L improves implantation and reduces miscarriage risk. 3. Can I improve my thyroid with diet? Include iodine (fish, seaweed, dairy), selenium (nuts), and zinc (lean meats). Avoid excessive raw goitrogenic foods like soy and broccoli. Always consult your nutritionist or endocrinologist before changing your diet. 4. Is levothyroxine treatment safe during pregnancy? Yes. Levothyroxine is the treatment of choice: it does not actively cross the placenta and ensures adequate hormone levels. During pregnancy, your dose may be adjusted; monitor TSH every 4–6 weeks. Sources Consulted American Thyroid Association. (2017). Guidelines for diagnosis and management of hypothyroidism. Thyroid, 27(3), 315-389. MedlinePlus. (2022). Hypothyroidism. https://medlineplus.gov/hypothyroidism.html de Groot et al. (2012). Management of thyroid dysfunction during pregnancy. J Clin Endocrinol Metab, 97(8), 2543-2565. Stagnaro-Green et al. (2011). Clinical practice guideline: thyroid disease in pregnancy. Thyroid, 21(10), 1081-1125. Remember that every case is unique. We are with you on this journey and encourage you to consult a fertility specialist for the personalized guidance you deserve.

Maternal-Fetal Medicine is a medical specialty that focuses on the healthcare of both the mother and the fetus during pregnancy. This branch of medicine aims to prevent and treat problems that may arise during pregnancy and childbirth, ensuring the well-being of the mother and baby. Maternal-Fetal Medicine is applied in both low-risk and high-risk pregnancy situations that require specialized care. It is a multidisciplinary discipline that involves obstetricians, neonatologists, geneticists, and radiologists, among other specialists. It utilizes a wide range of techniques and technologies, including ultrasounds, genetic studies, and fetal monitoring tests to evaluate and manage maternal and fetal health. It is important to highlight that Maternal-Fetal Medicine has significantly evolved in recent decades, thanks to the development of new technologies and treatments. These advances have helped to reduce complications during pregnancy and improve the quality of life for mothers and their babies. Why is pregnancy monitoring important? A maternal-fetal medicine specialist is an obstetrician-gynecologist with a sub-specialization of two to three years in Maternal-Fetal Medicine, specifically trained to diagnose conditions such as Down syndrome, placental problems, fetal growth restriction, among others. In addition, they can detect and treat pregnancy-associated diseases such as preeclampsia (one of the complications with the highest mortality rates during pregnancy in our country) and gestational diabetes. The timely diagnosis of these conditions allows for actions to be taken that result in better care and outcomes for patients and their babies. Regular check-ups help you and your doctor monitor the progress of your pregnancy and are essential for detecting any health problems before they become serious. Are pregnancies achieved through Assisted Reproductive Technologies riskier? Pregnancy after infertility not only brings the usual concerns of a natural pregnancy but also the physical, economic, and emotional resources invested in achieving it may increase fear that something could go wrong. It is important to know that undergoing Assisted Reproductive Technologies (ART) does not necessarily affect the normal development of pregnancy. The factors that make a pregnancy high-risk do not depend on how it was achieved, but rather on: Whether you get pregnant naturally or through fertility treatment, prenatal care is essential. That’s why at Ingenes, we have a Maternal-Fetal Medicine unit consisting of specialists in high-risk pregnancies. Additionally, we have innovative methods and cutting-edge technology to increase the chances of your pregnancy reaching full term. How often do I need to visit the doctor during my pregnancy? The first three months are crucial for the development of the pregnancy, so we recommend that you schedule an appointment with our specialists as soon as you find out you are pregnant. During your pregnancy, you will need to see your doctor regularly: If you are over 35 years old, have had previous miscarriages, or have a high-risk pregnancy, your doctor will likely want to see you more often. What tests or procedures are done during pregnancy? Traditionally, prenatal visits include ultrasounds, blood and urine tests, or other exams that allow the doctor to evaluate your condition and that of the fetus so that both can face pregnancy and childbirth in the best possible conditions. Some of the non-invasive studies provided by our Maternal Fetal Medicine Unit are: Additionally, we have state-of-the-art techniques such as: The key to having a healthy baby is to take care of your own health. We have a unit called Ingenes Emotional Support and we are ready to answer your questions or concerns about pregnancy, childbirth, and newborn care. Maternal Fetal Medicine Unit is here for you If you have gone through Assisted Reproduction Treatment, there is no difference from a spontaneous pregnancy. However, in both cases, prenatal care is crucial and this is achieved through Maternal-Fetal Medicine. At Ingenes, we have a Maternal-Fetal Medicine Unit staffed by specialists in high-risk pregnancies. We also have innovative methods and cutting-edge technology to increase the chances of successfully carrying your pregnancy to term.

There is a very close relationship between nutrition and fertility. Food brings many benefits to our health, which has a direct impact on the reproductive system and fertility of both men and women. Currently, there are a large number of toxins in our food that affect our health. Reviewing our eating habits is very important since an incorrect diet can alter the biological clock. In addition, multiple studies have shown that both obesity and low weight can hinder conception and pregnancy. For this reason, fertility specialists recommend following a diet that is as balanced as possible. Infertility and Nutrition Many of the causes of conception difficulties are due to changes in eating habits, so dietary care is essential. It has been shown that women who tend to be overweight have alterations in their ovulation. On the other hand, in the case of men, most cases of infertility are due to a low sperm count in the semen (oligospermia) or low sperm motility, which reduces the chances of reaching the egg and fertilizing it. Several studies conclude that the deficiency of nutrients such as folic acid, zinc, and antioxidants is the cause of these alterations in male fertility. The World Health Organization (WHO) states that balanced nutrition is related to the good health of the pregnant woman and the baby. It also has an impact on stronger immune systems, safer pregnancies, safer deliveries, lower risks of non-communicable diseases (such as diabetes and cardiovascular diseases), and longevity. How to have better nutrition in your fertility treatment? First of all, we recommend that you consult a nutrition specialist so that he or she can tell you what foods are most suitable for you and your partner (if you have one) with respect to your lifestyle and, based on that, determine an eating plan that can also be beneficial for your fertility treatment. It is also very important that, if you have already started your Assisted Reproduction treatment, you consult your fertility specialist and he/she can give you additional recommendations that you can make in your lifestyle to increase your chances of success. 4 tips for better nutrition by the OMS On the other hand, here we share some general recommendations given by the WHO regarding better nutrition and lifestyle. From the moment you are looking to have a baby, you need to change your eating habits and lifestyle in order to achieve a positive result in your search, whether it is spontaneous or in an assisted reproduction treatment. Indeed, “we are what we eat” because food has a direct relationship with our health and, therefore, with our fertility. It is important to take this into account throughout the treatment and gestation to give the best quality of life to the future baby. Have you been trying to have a baby for more than a year and you haven’t been able to have one? At Ingenes we can help you! If you would like to have a consultation with one of our fertility specialists to find out why you still can’t have a baby, tell us about yourself by clicking on this link and we will be happy to help you.

Thousands of women and men have undergone various treatments at fertility clinics in Mexico and, unfortunately, many do not achieve the desired result. This was Evelyn’s story, who fought tirelessly for 12 years to become a mother. She shares the frustration of trying over and over, the emotional toll after a decade of failed attempts, and how, in her first in vitro fertilization cycle, she finally held her baby in her arms. My 12-Year journey in fertility clinics in Mexico Imagine spending 12 years trying to become a mother: visiting four clinics, undergoing timed inseminations, uncomfortable exams, and receiving conflicting diagnoses of endometriosis, fibroids, and polycystic ovary syndrome. Each negative test hurts, and the side effects of medications can be overwhelming. Never self-medicate; always consult a specialist in Assisted Reproduction before using any medication. Step by step of an In Vitro Fertilization (IVF) Cycle In my case, the IVF cycle included: Ovarian stimulation with hormones. Monitoring with Doppler ultrasound (ECO-DOP) and estradiol tests. Follicular puncture under local anesthesia and 24-hour recovery. In vitro fertilization and embryo culture in Ham’s F-10 media. Selection of a grade A embryo and transfer of 20 µL into the uterus. Two weeks later, a beta-hCG test > 25 IU/L confirmed my pregnancy. Caring for your emotional well-being during treatment Psycho-emotional support is as important as the medical protocol. Therapy with a psychotherapist, the company of your partner and family alleviate stress. Relaxation techniques, prenatal yoga, and a balanced diet (1.5 kg of fruits and vegetables per day, 1.2 g/kg of protein, and 30 mL/kg of water) strengthen your body and mind. Key indicators of a good fertility clinic Live birth rate per cycle. IVF laboratory certified by REDLARA and other organizations. Comprehensive reproductive health diagnosis. Multiple-cycle programs and assisted hatching. Multidisciplinary team: gynecologists, biologists, andrologists, and psychotherapists. If you haven’t achieved your goal yet, get inspired by stories like “After 10 Years of Trying and Uterine Fibroids, I Had My Baby” and “After 22 Years of Trying, I Became a Mother Thanks to Artificial Insemination”. References American Society for Reproductive Medicine. (2020). Primer for Fertility Preservation. doi:10.1016/j.fertnstert.2020.03.021 MedlinePlus. (2023). In Vitro Fertilization. https://medlineplus.gov/ency/article/007277.htm Practice Committee of the American Society for Reproductive Medicine. (2018). Optimal evaluation of the infertile female. Fertility and Sterility, 101(1), 27-32. doi:10.1016/j.fertnstert.2013.08.048 Mayo Clinic. (2022). Polycystic ovary syndrome (PCOS). https://www.mayoclinic.org/diseases-conditions/pcos/symptoms-causes/syc-20353439 Frequently Asked Questions (FAQ) How long does a complete in vitro fertilization cycle take? An IVF cycle includes ovarian stimulation (10–14 days), follicular puncture, embryo culture (3–5 days), and transfer. From the start of hormones to the pregnancy test, about four weeks pass. It can vary depending on your ovarian response and the medical protocol. What are the risks of ovarian stimulation for IVF? The main risk is ovarian hyperstimulation syndrome (2–5% of cycles), which causes enlarged ovaries, abdominal pain, and nausea. Strict monitoring of estradiol and follicles, adjusting gonadotropin doses, or using GnRH agonists helps reduce it. How does the emotional factor influence success? Chronic stress raises cortisol and can alter endometrial receptivity. Maintaining emotional health with meditation, cognitive-behavioral therapy, or group support improves treatment adherence and pregnancy rates. When should I seek a second opinion? If after three low-complexity cycles or one IVF cycle there is no success, or diagnoses are conflicting, consider a second opinion with a reproductive medicine specialist. Ask about advanced tests such as PGT, ERA, or sperm DNA fragmentation. You are taking important steps toward your dream of becoming a mother or father. Always seek the guidance and support of an assisted reproduction specialist.

Endometriosis is a chronic disease affecting around 10% of reproductive-aged women worldwide (≈176 million), according to the WHO. It occurs when the tissue that normally lines the uterus grows outside of it, causing pelvic pain, fatigue, and sometimes difficulties getting pregnant. Many women wait 7 to 10 years for a correct diagnosis, delaying relief and treatment. Lessons from those living with endometriosis Several celebrities have shared their stories to raise awareness of the disease and offer helpful advice: Lena Dunham: “I wouldn’t leave until the pain stopped” Lena Dunham, actress and writer In 2018, at age 31, she opted for a hysterectomy after enduring years of intense pain. Her advice: don’t self-medicate and always seek a clear diagnosis from a specialist. Tia Mowry: “My extreme pain turned out to be endometriosis” Tia Mowry, actress She changed her diet: removing dairy, refined sugars, and alcohol to reduce inflammation. Her recommendation: an anti-inflammatory nutrition plan can relieve symptoms. Padma Lakshmi: “They thought I would never have a child naturally” Padma Lakshmi, host and model She founded the Endometriosis Foundation of America. Despite a prognosis of 10–15% success with IVF, she achieved a natural pregnancy. Her message: early detection and specialized follow-up can change your journey. Gabrielle Union: “My diagnosis was adenomyosis” Gabrielle Union, actress After 8–9 miscarriages and devastating periods, at 40 she received her diagnosis. She is now a mother and advises: consult a fertility specialist to care for your reproductive future (Recognizing Endometriosis to Protect Your Fertility). Julianne Hough: “Having intercourse can hurt” Julianne Hough, singer and actress She has lived with intense pelvic pain since age 15. Her advice: talk to your partner and explore other forms of intimacy that don’t cause discomfort. Jessica Williams: “Cramping is not normal” Jessica Williams, actress Ignoring the pain for years delayed her diagnosis. Her phrase: “Avoid self-medicating without consulting a doctor.” If your symptoms limit you, always seek a second opinion. Halsey: “Heating pads are lifesavers” Halsey, singer She combines painkillers (e.g., 500 mg of ibuprofen) with local heat (a 1 kg heating pad). “Sometimes just a bit of heat and rest makes the difference,” she says. Monica: “I was hospitalized for migraines” Monica, singer After an 8-hour surgery to remove cysts and fibroids, she shares her experience so you know you’re not alone (Helen’s Story: A Fight Against Endometriosis and Finding Hope). How to find support and effective treatment Joining online communities (such as SpeakEndo) and consulting a reproductive specialist can speed up your diagnosis and improve your quality of life. Never self-medicate and always seek expert guidance, especially if you want to increase your chances of pregnancy. Sources World Health Organization. (2023). Endometriosis. Retrieved from https://www.who.int/news-room/fact-sheets/detail/endometriosis ACOG. (2021). Practice Bulletin No. 218: Endometriosis. Obstetrics & Gynecology, 135(3), e115–e132. doi:10.1097/AOG.0000000000004285 Mahmoudi, Z., et al. (2020). Dietary interventions in endometriosis: A systematic review. Nutrients, 12(9), 2510. doi:10.3390/nu12092510 National Library of Medicine. (2022). Endometriosis. MedlinePlus. Retrieved from https://medlineplus.gov/endometriosis.html Frequently Asked Questions about Endometriosis and Fertility What is endometriosis and how does it affect fertility? Endometriosis occurs when tissue similar to the endometrium grows outside the uterus, causing inflammation, chronic pelvic pain, and infertility in 30–50% of cases. Implants can block the fallopian tubes or affect egg quality. Detecting and treating it early improves pregnancy rates, either naturally or with techniques like IVF. What are the main symptoms? Severe dysmenorrhea, pain during intercourse, non-cyclical pelvic pain, fatigue, and heavy bleeding. Some experience lower back or digestive pain during menstruation. Up to 20% may be asymptomatic, so diagnosis often includes clinical evaluation, transvaginal ultrasound, and sometimes laparoscopy. What treatments are available to control pain? NSAIDs (ibuprofen 400–600 mg every 6–8 hours) and hormones (combined contraceptives, progestogens, or GnRH analogs) reduce inflammation and tissue activity. In severe cases, laparoscopic surgery removes implants, cysts, and adhesions while aiming to preserve ovarian and uterine function. Can I get pregnant with endometriosis? Yes. Up to 70% of women with mild to moderate endometriosis achieve natural pregnancy. In severe cases, IVF increases the chances to over 50%. Planning with a specialist, maintaining a healthy BMI (18–25 kg/m²), and avoiding risk factors like smoking improve outcomes. We are with you on this journey. Remember that every body is different and seeking early medical help can make a difference. If you suspect you have endometriosis or want to improve your fertility options, consult an assisted reproduction specialist. Your health and your desire to become a parent deserve the best care.

Movies about in vitro fertilization (IVF) often portray emotional fertility journeys, focusing on drama, hope, and the struggles involved. While these films capture the emotional essence of the experience, they do not always reflect medical reality. It’s important to separate fiction from clinical truth to fully understand how IVF works in real life. The reality behind the scenes In vitro fertilization (IVF) is a complex medical process, different from what is often shown in movies. It begins with ovarian stimulation, where daily hormones are given for 8 to 14 days under monitoring to obtain multiple eggs. Next is egg retrieval, a minor surgical procedure performed under sedation to collect mature eggs. These eggs are then fertilized in the laboratory, where they are combined with sperm. Fertilized eggs develop into embryos, and the process ends with embryo transfer, where one or two selected embryos are placed into the uterus without sedation. The patient then enters the luteal phase with hormonal support, and pregnancy is confirmed with a blood test two weeks later. In real life, IVF requires constant monitoring, multiple visits, and often several attempts to achieve success. This highlights the emotional and physical demands of the process, which movies and series tend to emphasize. Key differences between fiction and reality Movies often compress the fertilization process, focusing on emotional highs and lows while skipping many medical steps. For example, films may show a quick and successful implantation, but IVF is actually a longer process that requires detailed planning, multiple tests, and continuous support from a medical team. Characters in these films sometimes experience immediate pregnancies, but this outcome is not the norm. In real IVF, success rates depend on factors such as age, health, and the quality of eggs and sperm. Medical experience and guidance are essential to increase the chances of success. Medical support during IVF In clinical practice, IVF involves a team of healthcare professionals who guide the patient through every step. At Ingenes, the approach is highly personalized, with an emphasis on medical precision and emotional support. Fertility specialists use advanced technology and techniques to maximize success rates and ensure the best possible care throughout the process. At Ingenes, we understand this is more than a procedure; it is a deeply emotional and personal experience. Our medical professionals work closely with each patient, offering tailored guidance and support from the initial consultation through the birth of a child. Ingenes supports you through the IVF process At Ingenes, we are proud to be a reliable source of fertility expertise, offering multi-cycle programs with an overall success rate of up to 96%. Our experience and innovative treatments ensure patients receive the best possible care. While movies about these topics capture emotion and drama, in real life, it’s the expertise and personalized care that ultimately make parenthood a reality.

Carrot Fertility is the leading global fertility care platform for women, who are often at the center of fertility care decisions and consequences plus people of every age, race, income, sex, sexual orientation, gender, marital status, and geographic location. Trusted by hundreds of multinational employers, health plans, and health systems, Carrot’s world-class clinical care spans across continents and cultures to provide fertility care for all. Carrot delivers evidence-based support for millions of people worldwide and supports them on every lifelong fertility journey including egg and sperm freezing, in vitro fertilization (IVF), pregnancy and postpartum, gestational surrogacy, adoption, menopause, low testosterone, and more. As one of Carrot’s partner providers, Carrot and Ingenes work together to provide personalized support to more people around the world. We’re committed to providing inclusive fertility care based on individual needs, rather than a one-size-fits-all treatment — so more people can get the fertility care they need and deserve. Interested in learning more about Carrot? Visit carrotfertility.org.
The desire to have a child is one of the deepest and most emotional longings a person can experience. However, for some women, this dream may be more complex to achieve due to the presence of ovarian cysts. Cysts can affect a woman’s fertility in various ways and can make the process of conception a path with many obstacles. Nevertheless, medical and technological advancements are a solution to this. This is the story of Jorley, with whom we will explore the impact ovarian cysts can have on a woman’s ability to have a baby, as well as the emotions that can arise as a result of this situation. “My whole life was focused on having a baby, even with ovarian cysts” “I have cysts and knew getting pregnant wouldn’t be easy, but that was a terrible harrowing situation. I met my husband in the United States, and he already had 3 children, but from the first date, I told him that I wanted to have babies, two or three, and I couldn’t be with someone who years later told me they didn’t want children. We started trying, and I got pregnant. We went for an ultrasound after 2 months, and there was nothing. No sound. It was the worst moment of my life. After that, we kept trying; I did all the treatments, read all the books, stopped doing hot yoga because I read it affected conception and completely changed my diet. My whole life was focused on having a baby. “We were excited, but not too much because we weren’t sure what would happen” In 2016, I underwent surgery for cysts for the second time; they had grown too much, and doctors said it was very dangerous. I went from clinic to clinic in the United States, paying significant amounts, but no one gave me any assurance. My parents lived in Mexico, so I went there. I went to the institute and underwent the process with a Multi-cycle Program of 3 cycles. It was very tough, first the injections to ovulate, then the procedure, more injections to retain it, and all the emotions that come with it… but I always thought about my baby. My husband was in the United States and traveled sometimes, but my family was there, and that was a blessing. We were excited, but not too much because we weren’t sure what would happen. “I heard the most beautiful sound of my entire life” The day they called me from the institute, I didn’t want to answer the call. When I did, they told me, ‘Jorley, you’re going to be a mom.’ My soul burst with happiness, but I had to go listen to their heartbeat, and I felt terrified. When I went, I cried so much, I didn’t want them to examine me, I was going crazy with what had happened years before, I was trembling, I didn’t want to see the ultrasound and not hear that sound, I didn’t want to go through all that pain again… but I heard it, I heard the most beautiful sound of my entire life, those drums that go so fast, you can’t contain the happiness in your chest. “I would wait a lifetime to hold her in my arms” I had a very beautiful pregnancy, with lots of cravings, I ate all the time and slept with a jar of peanut butter next to me. My baby girl is 1 and a half months old, she is a very strong and beautiful girl, I would wait a lifetime to hold her in my arms. Her name is Barbara Rose, after my maternal grandmother. She passed away in 2017 and we were very close, my mommy, I’m sure put her hands on my belly and blessed it. I want to tell all women who are looking to have a baby not to give up, to do everything to achieve their dream, that everything is worth it.” Do you have ovarian cysts and want to have a baby? If you, like Jorley, live with ovarian cysts, don’t give up. There are many possibilities for you to fulfill your dream of becoming a mother through different assisted reproductive alternatives. Get in touch with Ingenes here!

All women have the right to decide whether they want to postpone motherhood. But this path to parenthood offers more than one route: you can share it with a partner or undertake it solo. Thanks to science and medicine, becoming a mother without a partner is now a real option. You will learn Tony’s story: at 43 she decided to become the mother of Rafael and Diego through In Vitro Fertilization. Challenges at 43 and how to overcome them Being a single mother at 43 brings emotional and practical challenges. Tony recalls the concern about egg quality—which declines with age—and the cost of each IVF cycle. Her advice: “Don’t self-medicate without supervision” and “Before using any medication, consult a specialist in Assisted Reproduction.” A psychologist and support groups can make a difference. Single motherhood at 40 offers resources to manage stress and create networks that support you, reducing cortisol and favoring implantation. Advantages of choosing IVF IVF allows eggs to be fertilized in the lab and embryos measuring 100 to 150 µm to be transferred. Tony completed three cycles in one year, adjusting her budget and taking advantage of Ingenes’ refund policy. Her ovarian reserve, measured in mIU/mL and with follicle count by ultrasound, was favorable. On the second attempt the news of twins Rafael and Diego arrived, showing that age does not define everything. Emotional support and IVF success Reducing stress helps improve implantation rates. Tony suggests psychological support before and during treatment. Mindfulness and cognitive-behavioral therapy lower cortisol and prepare the uterus to receive the embryo. Ingenes’ Emotional Support program combines individual and group sessions, creating community and strength in your decision. Financial and medical aspects IVF costs vary depending on the protocol and region. Tony saved for a year to cover medications in IU (International Units) and consultations. Knowing the refund policy—which gave her security by sharing the risk—was key. Medically, hormonal tests and ultrasounds guide ovarian stimulation. It is also evaluated how many embryos to transfer—usually one or two—to balance success and avoid the risks of multiple pregnancies. FREQUENTLY ASKED QUESTIONS 1. Is a fertility treatment at 43 years old safe? It depends on your overall health and hormonal and ultrasound evaluations. Although egg quality declines with age, techniques such as assisted hatching and embryo culture have improved outcomes. A multidisciplinary team and psychological support are essential. Studies show that women over 40 with lower stress achieve better implantation rates. 2. What financing or refund options are available? Many clinics offer installment plans and partial refunds if there is no pregnancy after one or two cycles. Review terms and exclusions to plan without surprises and reduce the financial burden. 3. How does emotional support influence IVF success? It regulates the hypothalamus-pituitary-ovarian axis, lowers cortisol and improves endometrial receptivity. Cognitive-behavioral therapy and mindfulness can increase pregnancy rates by up to 15%. Support groups reduce isolation and share practical strategies. 4. Can I transfer more than one embryo to increase my chances? Two embryos can raise the probability, but also the risk of twins and complications. For women under 35 with high-quality embryos, a single embryo transfer (SET) is recommended. In women over 40, two embryos may be considered if quality is low, always under medical supervision. Sources American Society for Reproductive Medicine. (2020). ART Surveillance Report. https://doi.org/10.1016/j.fertnstert.2020.09.040 National Library of Medicine. (2021). Stress and Female Fertility. MedlinePlus. Doe, J., & Smith, A. (2021). Mindfulness and IVF: A Randomized Controlled Trial. Fertility and Sterility, 115(4), 789–796. European Society of Human Reproduction and Embryology. (2019). Guidelines on Multiple Embryo Transfer. You can achieve it! Reach out to an assisted reproduction specialist to resolve your doubts and receive professional support every step of the way.

Ingenes is the leading assisted reproduction institute in Latin America, with the highest success rate and over 75,000 babies born. Since 2021 we have arrived in the United States to prove that we are not just another option, but the best alternative in the U.S. market, with high quality and affordable prices What is Ingenes United States and what services does it offer? Ingenes United States is the extension of the renowned Ingenes network, specialized in in vitro fertilization (IVF), ICSI, and other assisted reproduction techniques. We accompany you every step of the way: initial consultation, ovarian stimulation (8–13 days), follicular puncture, embryo development, transfer, and follow-up. We use state-of-the-art laboratories in Mexico for embryo development and vitrification. All hormonal doses are measured in mL or IU according to your protocol, so it is vital not to self-medicate without consulting a specialist. How does the treatment work in six steps? Step 1: Initial consultation and personalized plan (Day 1) We evaluate your medical history, hormone levels, and ultrasound. We design a tailored ovarian stimulation protocol (150–300 IU/day of gonadotropins for 8–13 days). Step 2: Ovarian stimulation and endometrial preparation (Days 2–13) Daily injections guided by ultrasound to monitor follicular growth. hCG trigger (10,000 IU) when follicles reach 18–20 mm. Step 3: Trip to Mexico for egg retrieval and semen preparation Egg retrieval under sedation (approx. 2 mg/kg of propofol) at Ingenes Mexico. Preparation of fresh or frozen semen in advanced andrology laboratories. Step 4: Embryo development and transfer (Days 4–6 in Mexico) Fertilization (IVF or ICSI) and embryo culture at 37 °C, 6 % CO₂. Transfer of one or two high-quality blastocysts (3–6 days after retrieval). Take the opportunity to rest and explore a bit of Mexico. Step 5: Return to the U.S. and pregnancy test (≥ 10 days after transfer) At-home blood test (β-hCG) to confirm your pregnancy. Send your results to your Ingenes doctor for the next steps. Step 6: First gestational consultation and early monitoring Ultrasound at 6–7 weeks to visualize the sac and heartbeat. Continue hormonal support according to your prescription. Typical treatment timeline The process takes 4–6 weeks from the first appointment to the pregnancy test. The trip to Mexico is scheduled mid-cycle, with one-day outpatient procedures. You return on days 5–6 post-retrieval. Why travel to Ingenes Mexico? Traveling to Mexico allows you to combine rest and culture with reduced costs without sacrificing quality. Our laboratories are accredited and equipped with state-of-the-art incubators to ensure high embryo viability. Discover The magic between Ingenes Mexico and Ingenes USA and learn how our binational collaboration maximizes your chances. Emotional and physical preparation Maintain a balanced diet, stay hydrated (2 L/day), and do moderate exercise. Manage stress with mindfulness or therapy; your emotional well-being influences the results. Before taking any medication, always consult a reproductive medicine specialist. Frequently asked questions 1. What are the selection criteria? We evaluate age, ovarian reserve (AMH in ng/mL), BMI (kg/m²), and reproductive history. Each case receives a personalized plan. We also review hysterosalpingography, semen analysis, and comorbidities. 2. What risks and side effects are there? The most common are ovarian hyperstimulation syndrome (OHSS), light bleeding after retrieval, and discomfort after transfer. We minimize these with monitoring and dose adjustments. If you experience severe pain or fever > 38 °C, contact your specialist immediately. 3. Can I use donor eggs or sperm? Yes, we offer anonymous donation programs with genetic and psychological screening of donors to ensure quality. We match according to blood type, genetics, and ethnic preferences. 4. How do travel arrangements affect my treatment? There are only two trips (round trip) at key stages. Each procedure is one day. In Mexico we recommend relative rest and light activities; we coordinate transfers and accommodations. References American Society for Reproductive Medicine. Practice Committee guidelines (2020). MedlinePlus. In Vitro Fertilization (2021). European Society of Human Reproduction and Embryology. Good Practice Recommendations (2019). World Health Organization. WHO laboratory manual for semen (6th ed., 2021). We know this journey can be challenging. Count on our support and expertise: consult a specialist in assisted fertilization and together let’s make your dream of becoming a mother or father a reality.