Don't miss our updates


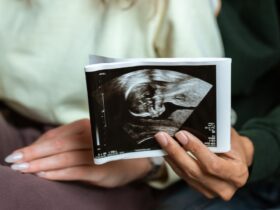
The journey to parenthood is unique for each couple, and an accurate diagnosis is the essential first step. At Ingenes, we understand that every detail counts on the path to having a baby at home. The Importance of an Accurate Medical Diagnosis An accurate medical diagnosis is essential to chart a clear path in fertility treatment. Correctly identifying the causes of infertility not only makes it easier to select the most appropriate treatment but also gives couples a deeper understanding of their situation. This is crucial to managing emotions and expectations during this process. The Five Pillars of Fertility The Importance of a Timely Diagnosis A timely and accurate diagnosis can be the difference between years of unsuccessful treatments and a successful path to motherhood. At Ingenes, 90% of our patients arrive after having gone through exhausting experiences, both physically and emotionally. Therefore, our focus is on avoiding the loss of valuable time and providing fast and accurate diagnoses. Technology and Expertise at Ingenes We have cutting-edge technology and a team of highly trained specialists in various areas of assisted reproduction. This allows us to offer a clear diagnosis and a personalized treatment plan from the first consultation. Understanding and Managing Infertility Understanding the causes of infertility and the details of treatment helps couples better manage the situation. At Ingenes, we strive to provide not only medical advice but also emotional support, so that each couple feels safe and understood at every stage of the process. At Ingenes, your dream of having your baby at home is our priority. We understand that the path to fertility can be complicated, but with an accurate diagnosis and proper treatment, we are here to help you turn that dream into reality. If you are looking to have a baby at home and want to better understand your fertility situation, visit Ingenes. Our experts are ready to guide you every step of your journey. Contact us today to start your path to parenthood.

Infertility knocks on many doors and affects not only couples but also those around them. At Ingenes we understand this situation and know that the love and support of those around you make all the difference. How can family and friends truly support? When someone you care about faces infertility, the desire to help is huge, but sometimes words or actions miss the mark. To offer heartfelt support: Listen without judging More than giving advice, create a safe space. Let them express their fears, dreams, and frustrations. An “I’m here for you” can ease more than any solution. Respect their privacy They may not want to share every detail of their treatment. If they speak, respond with empathy; if they prefer silence, honor that. Practical actions that make a difference Details matter. A few ideas: Help with daily tasks Prepare ready-to-serve meals (250 mL of soup or stew in 500 g portions). Pitch in with household chores; 15 minutes of tidying can boost morale. Accompany them to medical appointments, especially if they’re on an IVF protocol with 150 IU gonadotropin injections. Invite them gently Suggest going out or gathering, but make it clear they can say no without any problem: “If you’re not up for it today, I completely understand.” Why is understanding infertility key? Infertility is more than a medical issue; it’s an emotional journey. By learning from reliable sources like Ingenes treatments, you can offer informed, empathetic support. Avoid unsupervised medicines. Before trying any treatment or supplement, consult an assisted reproduction specialist. Impact of emotional support on treatments Studies show that a strong support network reduces stress and lowers cortisol by up to 25%, which helps balance reproductive hormones. Feeling accompanied makes the process more bearable. Frequently Asked Questions How Do I Talk to Someone Facing Infertility? Ask open-ended questions: “How are you feeling today?” instead of unsolicited advice. Acknowledge their emotions: “This must be really hard for you.” That builds trust. Avoid phrases like “just relax.” Offer concrete help: “Can I drive you to your next appointment?” A simple gesture shows you care without minimizing their experience. Can I Ask About Their Progress? Express interest, but let them set the pace: “I’m thinking of you. If you want to share how things are going, I’m here to listen.” If they prefer not to talk, respect their choice: “I understand. Whenever you’re ready, I’m here.” This shows your support is unconditional. What Should I Avoid Saying? Skip clichés like “everything happens for a reason” or “at least you have each other.” They can sound empty. Better say: “I can’t imagine what you’re going through, but I care about you deeply.” Don’t compare or share medical anecdotes. Every journey is unique; listen and respond with empathy. How to Support During Treatments? Offer to accompany them to appointments, help manage medication schedules (for example, remembering 0.1 mg daily of a supplement), or simply be present. Sometimes minutes of silent company are enough. Send meaningful details: a handwritten note, a relaxing playlist, or a 250 mL scented candle. Gestures like these say “I’m thinking of you.” Sources Consulted American Society for Reproductive Medicine. (2021). Infertility FAQs. Fertility and Sterility, 115(3), 567-576. https://doi.org/10.1016/j.fertnstert.2020.09.019 MedlinePlus. (2022). Infertility. U.S. National Library of Medicine. https://medlineplus.gov/infertility.html Pasch, L. A., Holley, S. R., & Bleil, M. E. (2020). Stress and infertility: A review. Journal of Psychosomatic Obstetrics & Gynecology, 41(3), 132-141. https://doi.org/10.1080/0167482X.2020.1756074 World Health Organization. (2018). Infertility definitions and terminology. WHO Reproductive Health Library. You are not alone on this journey. If you or your partner are seeking to increase your chances of pregnancy, consult an assisted fertilization specialist. We are here to support you.
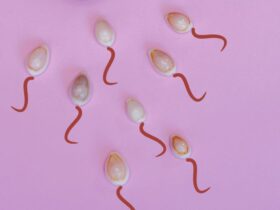
The seminal tract is the path that sperm take from the testes to the outside. If an infection occurs at any point along this route, the inflamed areas can damage semen quality and make it harder for the egg to be fertilized. The good news is that most of these infections respond very well to antibiotics. If semen quality remains low after treatment, in vitro fertilization with ICSI is usually the best option to achieve pregnancy. What are seminal infections and how do they affect your fertility? Seminal infections arise when bacteria, fungi, or viruses reach the prostate, seminal vesicles, epididymis, or vas deferens. This can cause: Obstruction of seminal flow, causing azoospermia (absence of sperm) or oligozoospermia (fewer than 15 million/mL). Reduced sperm motility (asthenozoospermia). Abnormal sperm morphology (teratozoospermia). Increased sperm DNA fragmentation, making implantation more difficult. Production of antibodies against sperm. Possible transmission of the infection to your partner. What are the symptoms? They are often silent and only detected through a fertility study, but sometimes they present with: Changes in semen color or consistency. Irritation, itching, or burning when urinating. Urethral discharge. Discomfort in the perineal or testicular area. Avoid self-medication. If you notice any of these symptoms, stop sexual activity and consult an assisted reproduction specialist. Why do they occur? The most common causes are sexually transmitted bacteria (Chlamydia trachomatis, Neisseria gonorrhoeae) or intestinal flora (such as Escherichia coli or Enterococcus faecalis). The risk is higher with unprotected sex or multiple partners. Factors that increase the likelihood: Poor genital hygiene. Invasive urological procedures. Weakened immune system. How is it diagnosed? The specialist usually: Takes your medical history and performs a physical exam. Performs a urine culture and semen culture with antibiotic sensitivity. Orders molecular tests (PCR). Analyzes the semen with a semen analysis and DNA fragmentation test. With this information, a personalized treatment plan is designed and follow-up studies are performed to confirm that the infection has cleared. Treatment and options for achieving pregnancy Initial treatment is usually oral antibiotics for 7–14 days. It is essential that both you and your partner complete the course and maintain sexual abstinence during the medication period. Once the infection is eradicated, sperm quality is reassessed. If problems persist (concentration < 15 M/mL, motility < 40%, or high fragmentation), IVF+ICSI or additional tests in our fertility laboratory are considered. Frequently Asked Questions 1. Do they always cause infertility? No. Many are detected and treated in time, restoring semen quality. However, if inflammation becomes chronic, it can cause scarring and blockages, leading to persistent oligozoospermia or asthenozoospermia. Consult as soon as you notice any symptoms. 2. Can I infect my partner during treatment? Yes, which is why both partners should be treated simultaneously. Abstinence and condom use after therapy help prevent reinfection. 3. How does DNA fragmentation affect things? If it exceeds 30%, it can hinder natural fertilization and increase the risk of miscarriage. In those cases, ICSI along with prior antioxidant supplements is recommended. 4. Can they be prevented? With safe sexual practices (condom use), good genital hygiene, and regular check-ups if you have risk factors. A healthy lifestyle (balanced diet, exercise, no smoking) also strengthens your immune system. Sources National Library of Medicine. (2023). Male reproductive system infections. MedlinePlus. https://medlineplus.gov World Health Organization. (2021). WHO laboratory manual for the examination and processing of human semen (6th ed.). Geneva: WHO Press. Dohle, G. R., Diemer, T., Kopa, Z. (2019). EAU Guidelines on Male Infertility. European Urology, 76(4), 616–628. https://doi.org/10.1016/j.eururo.2019.08.029 Esteves, S. C., Agarwal, A. (2020). Role of oxidative stress in male infertility. Clinics, 75, e1909. https://doi.org/10.6061/clinics/2020/e1909 Remember that each case is unique. If you are looking to start a family, do not hesitate to consult an assisted reproduction specialist: we are here to support you every step of the way.

Anovulation is the absence of ovulation that occurs when the ovaries do not release eggs. It is usually due to hormonal imbalances and is one of the most common causes of fertility problems. Any fertility treatment should be accompanied by hormone therapy with estrogen and progesterone to prepare the endometrium for embryo implantation with assisted reproductive techniques. Patients with anovulation should be referred to an assisted reproduction institute where they can undergo ovulation induction treatment with medication. What is Anovulation? Anovulation is the absence of ovulation that occurs when the ovaries do not release eggs. It accounts for about 25 percent of female fertility problems and is generally due to hormonal imbalances caused by factors such as stress, eating disorders, excessive exercise, and polycystic ovary syndrome, among others. Main Symptoms of Anovulation The main symptoms of anovulation are: Because some women with anovulation continue to menstruate regularly, this condition can be difficult to detect. Causes of Anovulation Anovulation can be due to various disorders at the level of the hypothalamus, pituitary gland, or ovaries and is generally linked to hormonal imbalances. Factors such as stress, eating disorders, and excessive exercise can cause alterations in the hypothalamus, which under normal circumstances secretes gonadotropin-releasing hormone (GnRH). GnRH acts on the pituitary gland, stimulating its production of luteinizing hormone (LH) and follicle-stimulating hormone (FSH), which are essential for ovulation. Failures in communication between the hypothalamus and the pituitary gland can affect the hormonal function of the ovaries and lead to disorders such as polycystic ovary syndrome, which is the leading cause of anovulation. Other factors affecting ovulation include: How is Anovulation Diagnosed? In addition to a pelvic exam and a review of the patient’s medical history, procedures to diagnose anovulation may include: Once the diagnosis is obtained, the doctor may perform additional tests to determine the causes of anovulation. Treatments to Achieve Pregnancy in the Presence of Anovulation Any fertility treatment should be accompanied by hormone therapy with estrogen and progesterone to prepare the endometrium for embryo implantation with assisted reproductive techniques. Patients with anovulation should be referred to an assisted reproduction institute where treatments include: Each case is different, so it is essential to consult a fertility specialist who can help determine the best treatment for you.

Seeking professional help in time can make all the difference. Time directly influences the success of fertility treatments. Assisted reproduction offers multiple options and technologies. Success depends on an accurate diagnosis and choosing the treatment that best fits your case. When choosing a clinic, review its pregnancy rates, the experience and credentials of the medical team, the quality of its facilities, and its national and international recognition. Choose a place where you feel listened to and supported, with clear and accessible information about every step of your treatment. When to seek fertility help? If you and your partner have been trying to conceive without protection for more than 12 months (or 6 months if she is over 35) or have experienced miscarriages, it’s time to consult. The WHO defines infertility as a woman under 35 not conceiving after 12 months of unprotected intercourse, or 6 months if over 35. Remember that infertility can also appear after having had children. According to the CDC, 11% of couples with previous conceptions experience infertility. Why does a woman’s age matter? After age 35, the chance of pregnancy with own eggs decreases. In women under 30, the natural cycle rate is 20–30%, but by 40 it drops to 5% and the risk of miscarriage and genetic abnormalities increases. Beyond age 42, conceiving with own eggs is rare. With donated eggs, many women become mothers past 50. At Ingenes you will receive a timely diagnosis and a personalized treatment plan. Comprehensive couple diagnosis Infertility affects men and women equally. A joint diagnosis ensures greater accuracy. In men, sperm concentration, motility, and morphology are evaluated through a semen analysis. Treatment options They range from medications like clomiphene (50 mg/day) to high-tech techniques. Having a clear diagnosis and knowing your alternatives is fundamental. You and your specialist will design a personalized plan to maximize your chances. How to choose your clinic Pregnancy success rates Team experience and training National and international recognition State-of-the-art facilities and technology Close, empathetic, and transparent care Ingenes, endorsed by Illinois Fertility Center and the Latin American Network for Assisted Reproduction, exceeds the U.S. success average. From your first visit you will have a clear diagnosis and an effective action plan. Improving your lifestyle also helps: quit smoking, moderate coffee and alcohol, maintain a healthy diet and weight. Stress affects fertility; our emotional support unit will accompany you at every stage. Visit Tips for Improving Fertility and prepare for your First Visit to the Clinic. Costs and financing Most insurance in Mexico does not cover these treatments. At Ingenes we offer flexible financing plans so nothing stops your dream of becoming a mom or dad. Success indicators Endometrial thickness (ideal ≥7 mm), estradiol and progesterone levels, your emotional well-being, and healthy lifestyle habits are key to a positive outcome. Frequently Asked Questions When Should I Evaluate My Fertility? If you are under 35 and have been trying for 12 months without success (6 months if over 35), consult a specialist. Early diagnosis saves time and stress and allows you to create an effective plan from the start. How Does Age Affect Fertility? Fertility declines after 35. By 40, the chance of conceiving with own eggs is 5% per cycle and genetic risk increases. A prompt evaluation and, if needed, using donated eggs can change your path to motherhood. What Does a Semen Analysis Evaluate? It analyzes sperm concentration, motility, and morphology. A normal result rules out male causes; abnormalities guide toward specific techniques like IUI or IVF with personalized outcomes. Emotional Preparation for Treatment Stress and anxiety affect fertility. Psychological therapy, support groups, and relaxation techniques reduce tension and improve treatment adherence. At Ingenes, our emotional support unit will provide strategies and continuous accompaniment. Sources Centers for Disease Control and Prevention. (2023). Infertility FAQs. https://www.cdc.gov/reproductivehealth/infertility/index.htm World Health Organization. (2022). Infertility definitions and treatment. https://www.who.int/news-room/fact-sheets/detail/infertility Practice Committee of the American Society for Reproductive Medicine. (2021). Diagnostic evaluation of the infertile female: a committee opinion. Fertility and Sterility, 116(2), 318–327. https://doi.org/10.1016/j.fertnstert.2021.03.042 American Urological Association. (2020). Male Infertility: AUA Guideline. https://www.auanet.org/guidelines/male-infertility-guideline We know how important this moment is for you. You are not alone on this journey. Consulting an assisted reproduction specialist will give you the support and guidance you need to fulfill your dream of becoming a mom or dad.

¿Se puede quedar embarazada con quistes en los ovarios? Conoce a Rosy, una mujer de más de 35 invadida de quistes, y cómo logró a su bebé.

Silvia fue mamá después de los 40 años con una Fecundación In Vitro, pero la gran sorpresa fue que año y medio después se embarazó de nuevo sin ayuda.
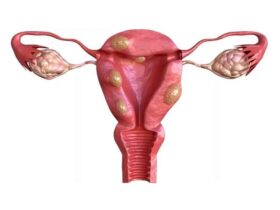
Uterine myomatosis is the formation of myomas or fibroids inside the uterus. These are benign tumors classified according to their location. Depending on where they are found, fibroids are classified as: Intramural: within the muscular wall of the uterus. They can affect fertility if they exceed 4 cm. Submucosal: on the surface of the uterine lining. They hinder embryo implantation. Subserosal: in the outer layer of the uterus. They usually do not interfere with fertility. What is uterine myomatosis and why does it matter for fertility? Uterine myomatosis involves the growth of fibroids, benign smooth muscle tumors, inside the uterus. It affects about 20% of women of reproductive age, especially after age 30. Fibroids can range from microscopic nodules to masses over 4 kg, altering the shape of the uterus and reducing pregnancy chances. How common is uterine myomatosis in those trying to conceive? Uterine fibroids are the most common pelvic tumors in women of reproductive age, present in nearly 70–80% before menopause. Although many are asymptomatic, those that deform the uterine cavity—particularly large intramural and submucosal fibroids—are involved in up to 80% of uterine factor infertility cases. How do fibroids affect embryo implantation? Large submucosal and intramural fibroids can: Alter sperm transport and uterine peristalsis Reduce endometrial receptivity by compressing the lining Increase the risk of implantation failure and early miscarriage Can fibroids complicate pregnancy? Yes. During pregnancy, fibroids can cause: Higher risk of miscarriage and preterm birth Fetal growth restriction due to lack of space Cervical canal obstruction or labor dystocia Postpartum hemorrhage from poor uterine contraction What symptoms may indicate fibroids? About 25% are asymptomatic. When symptoms occur, they include: Sensation of pelvic pressure or heaviness Heavy or prolonged menstrual bleeding Pelvic cramps and irregular bleeding Frequent urination or difficulty urinating Secondary infertility or recurrent miscarriages Severity depends on fibroid size, number, and location. How is diagnosis confirmed? Transvaginal ultrasound is the gold standard, with nearly 100% sensitivity (95% transabdominal). In complex cases, MRI is used. Always consult a reproductive medicine specialist to interpret results and design a treatment plan. Fertility-preserving treatment options Choice depends on age, fibroid characteristics, and reproductive goals: Expectant management for small, asymptomatic fibroids Myomectomy (surgical removal), followed by assisted reproduction techniques Controlled ovarian stimulation combined with in vitro fertilization (IVF) if cavity distortion persists IVF bypasses uterine transport obstacles and allows for selecting the embryo with the highest implantation potential. For more information, see our guide on Endometriosis: what it is and how it impacts fertility. FAQ 1. Can small fibroids disappear on their own? Yes. Many remain stable or shrink after menopause due to estrogen decline. In reproductive age, asymptomatic fibroids under 2 cm are usually monitored with periodic ultrasounds. If you plan to conceive, even a small submucosal fibroid can affect implantation, so consult your doctor to assess intervention before trying to conceive. 2. Are there non-surgical treatments? GnRH agonists and selective progesterone receptor modulators can temporarily shrink fibroids and reduce bleeding in 3–6 month cycles. They improve conditions before surgery or comfort but are not definitive solutions. Never self-medicate without medical supervision. 3. When can I attempt IVF after a myomectomy? Ideally between 6 and 12 months after surgery, before recurrence risk increases. This timing allows the uterine lining to heal and optimizes pregnancy chances. Make sure your specialist confirms proper healing with ultrasound or hysteroscopy before starting treatment. 4. Does the risk of miscarriage increase? Yes. Fibroids that deform the cavity or alter blood flow are associated with early pregnancy loss. Risk increases with fibroid size and location, especially submucosal and large intramural fibroids. Proper management, surgical or with assisted reproduction, significantly reduces miscarriage rates. Always consult a specialist before making decisions. References Faerstein, E., Szklo, M., & Schwingl, P. J. (2001). Risk factors for uterine leiomyoma: a practice-based case–control study. American Journal of Epidemiology, 153(5), 463–469. doi:10.1093/aje/153.5.463 Lau, W., & Shlisselberg, S. (2016). Management of uterine fibroids. American Family Physician, 94(2), 106–113. https://www.aafp.org/afp/2016/0715/p106.html MedlinePlus. (2021). Uterine fibroids. https://medlineplus.gov/uterinefibroids.html Stewart, E. A. (2015). Uterine fibroids. Lancet, 376(9745), 145–157. doi:10.1016/S0140-6736(10)60246-1 Remember: every body is unique. Stay informed, keep hope, and consult an assisted reproduction specialist for personalized care.

Michelle Obama’s brave revelation about her experience with pregnancy loss has touched the hearts of millions of women around the world. Her story is not only one of pain and loss but also one of resilience and hope. By openly sharing her journey through infertility, Michelle has shed light on a topic that often remains in the shadows, surrounded by stigma and silence. At Ingenes, we recognize the importance of these personal narratives and how they can inspire and encourage other women facing similar challenges in their desire to start a family. Michelle’s tragic experience highlights an issue that affects a surprisingly large number of couples around the world. Pregnancy loss, a deeply moving and life-changing event, can leave lasting emotional scars and unanswered questions. At Ingenes, we are committed to providing a safe and supportive space where these stories can be shared and where couples can find a sense of community and understanding. Our mission at Ingenes goes beyond offering cutting-edge fertility treatments. We strive to understand the emotional and physical complexities our patients face on their path to parenthood. Michelle Obama’s story not only motivates us to continue our work, but also reminds us of the importance of approaching these issues with sensitivity, care, and a deep respect for each person’s individual experiences. What lessons can we learn from Michelle Obama’s pregnancy loss? In “Becoming”, Michelle Obama shares the intimate details of her experience with miscarriage. This honest account reminds us that pregnancy loss affects 10–20% of known pregnancies and is often underreported due to stigma. By speaking openly, she has given voice to many women who feel alone in their grief and inspired them to seek support. How does In Vitro Fertilization work and when should it be considered? After their loss, the Obamas opted for In Vitro Fertilization (IVF). IVF involves retrieving mature eggs and sperm, combining them in a lab dish, and transferring viable embryos into the uterus. Success rates vary by age and clinic but can range from 30% to 50% per cycle. At Ingenes, we tailor protocols—dosing hormones in IU and monitoring follicle growth in mm—to optimize outcomes. Why is emotional support crucial during infertility treatments? Pregnancy loss and fertility treatments carry a heavy emotional toll. At Ingenes, we complement our medical protocols with counseling services, support groups, and mind–body therapies. Studies show that women who receive psychosocial support have higher treatment adherence and report reduced anxiety and depression. Our approach is rooted in empathy: we listen, validate your feelings, and accompany you at every step. How can personalized treatment plans improve fertility outcomes? Couples respond differently to medications and protocols. By analyzing AMH levels in ng/mL, antral follicle counts, and genetic factors, our team crafts individualized plans. Whether it’s adjusting the gonadotropin dose from 150 IU to 300 IU or selecting time-lapse embryo monitoring, personalization boosts implantation rates. Michelle Obama’s story is a source of inspiration and hope. At Ingenes, we strive to provide our patients with the best fertility care and treatments, helping them turn their dreams of becoming mothers into reality. For more success stories, explore Celebrities and In Vitro Fertilization: Stories of Success and Hope. Avoid self-medicating without consulting a doctor. Before resorting to this medication, you need to see a specialist in assisted reproduction, particularly if you are looking to increase your chances of getting pregnant. Frequently Asked Questions What are the most common causes of pregnancy loss? Chromosomal abnormalities in the embryo account for nearly 50% of miscarriages, especially in the first trimester. Other factors include uterine malformations, hormonal imbalances like low progesterone, thyroid disorders, or uncontrolled diabetes. Lifestyle factors—smoking, excessive caffeine, or obesity—can also increase the risk. How long should I wait after a miscarriage before trying again? Medical guidelines suggest waiting at least one to three regular menstrual cycles before attempting conception to allow the endometrium to recover and ensure accurate dating of a new pregnancy. Emotional readiness is equally important—seek counseling if feelings of grief or anxiety persist. When is it appropriate to consider assisted reproduction? Couples under 35 who have tried unprotected intercourse for 12 months without success, or women over 35 who have tried for six months, should be evaluated for infertility. Factors like low ovarian reserve (AMH

Uterine myomatosis is the appearance of fibroids or fibroids, the most common solid tumors of the uterus in women of reproductive age. They are generally benign estrogen-dependent tumors. They are also called myoma, leiomyoma, or fibroma.Epidemiologically, 2 out of 5 women who present with fibroids do not have any symptoms. They are not a common cause of infertility. For patients who have fertility problems, fibroids have a prevalence of 5-10%. Only in 1 to 2.5% of cases is it a cause of infertility. (1) Among the risk factors that contribute to the development of uterine fibroids are nulliparity, black race, obesity, genetic factors, early menarche, alcohol, and caffeine. (2) The classification of uterine fibroids is based on the relationship they have with the uterine wall, thus they can be subserosal, intramural, and submucosal. 95% of fibroids are located in the body of the uterus, and only 5% are located at the neck. Subserosal fibroids constitute about 10%, originate from the most superficial layers of the uterus, and appear to have no impact on fertility; Intramural fibroids constitute 60 to 70%, they generally do not distort the endometrial cavity, the effect on fertility is not clear or may be minimal when the endometrium is not involved. Submucosal fibroids have a frequency of 15 to 20%, they originate in the myometrium adjacent to the body or cervical uterine mucosa, exerting changes in it, they are the ones that most affect the chances of pregnancy and put an ongoing pregnancy at risk. (3) The symptoms caused by uterine fibroids are related to the location and size of the tumor. In most cases, women with fibroids are asymptomatic. The main symptoms that women report are menstrual disorders, generally with abundant and/or prolonged bleeding that can lead to anemia, pelvic pain, dysmenorrhea, dyspareunia, pelvic heaviness, urinary symptoms, or digestive symptoms. Women with submucosal fibroids more frequently have fertility problems or spontaneous abortions. The explanations are: The diagnosis is usually based on the finding of an enlarged, mobile uterus with irregular contours on physical examination or as an incidental finding on ultrasound. Imaging techniques are useful when it is necessary to confirm the diagnosis or locate the fibroid. Ultrasound is the most widely used diagnostic tool due to its availability and cost/effectiveness. Transvaginal ultrasound has a high sensitivity (95-100%) to detect fibroids in uteruses younger than 10 weeks. The sonohysterogram has greater sensitivity and specificity for submucosal fibroids since it detects the anatomical relationship between the fibroid and the uterine cavity. Magnetic resonance imaging gives better information on the origin of the fibroid. Hysterosalpingography is indicated to study the uterine cavity and the integrity of the uterine ruptures in patients with infertility. If the uterine cavity is normal, there is no advantage in performing a hysteroscopy. If the location of the fibroid is not clear in patients with abnormal uterine bleeding or in those seeking pregnancy, contrast-enhanced ultrasound (sonohysterogram) is the procedure of choice. If imaging studies do not provide an accurate diagnosis, surgical exploration is sometimes required. (5) The treatment of uterine fibroids can be divided into medical and surgical. Medical treatment is associated with inhibition of ovulation, reduction in estrogen production or modification in estrogen and progesterone receptors. Surgical treatment is indicated or recommended in patients with abnormal uterine bleeding that does not respond to medical treatment, high suspicion of malignancy, growth after menopause, infertility with distention of the endometrial cavity or tubal obstruction, pain or a sensation of pressure that interferes with good quality of life, urinary frequency obstruction or disorder, and anemia related to abnormal uterine bleeding. (6) New management presents an alternative to hysterectomy, both safety and effectiveness must be considered in each treatment. It must be recognized that all the new alternatives to hysterectomy allow the possibility of reappearance of undetected leiomyomas mainly because they are small, and may present significant growth, and require new treatment. The risk of recurrence must be balanced with the potential benefits of uterus-sparing procedures, such as decreased morbidity rates and fertility. (7) During the first visit, our patients receive a complete evaluation and adequate classification, mainly in patients with fibroids that involve the endometrial cavity through endovaginal ultrasound, sonohysterogram, and, if necessary, a hysteroscopy. Avoiding at all times unnecessary surgeries that do not contribute to the reproductive goal and/or that put the integrity of our patients at risk. If submucous fibroids < 3cm are present, patients should be managed hysteroscopically. Removing subserosal fibroids is not recommended since they do not contribute to improving the reproductive goal. Patient selection should be individualized based on number, size, and location in addition to the surgeon’s skills. (8) (1)-AAGL Practice Report: Practice Guidelines for the Diagnosis and Management of Submucous Leiomyomas, The Journal of Minimally Invasive Gynecology, 2012(2)- Donnez J, Uterine fibroids management:from the present to the future, Hum Reprod Update, Nov 2016.(3)-SOGC CLINICAL PRACTICE GUIDELINE, The management of uterine fibroids in women with otherwise unexplained infertility, March 2015.(4)-AAGL Practice Report: Practice Guidelines for the Diagnosis and Management of Submucous Leiomyomas, The Journal of Minimally Invasive Gynecology, 2012(5)-E., Pritts, Fibroids and Infertility: an updated systematic review of the evidence, Fertility and Sterility, april 2009.(6)-SOGC CLINICAL PRACTICE GUIDELINE, The management of uterine fibroids in women with otherwise unexplained infertility, March 2015.(7)-SOGC CLINICAL PRACTICE GUIDELINE, The management of uterine fibroids in women with otherwise unexplained infertility, March 2015.(8)-E., Pritts, Fibroids and Infertility: an updated systematic review of the evidence, Fertility and Sterility, april 2009
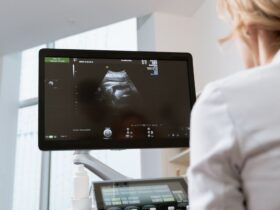
For couples dreaming of becoming parents, understanding the causes of infertility is a key step. An accurate diagnosis makes it possible for almost 98% of those dreams to come true. Endometriosis, if not detected in time, can place obstacles on your path to motherhood. What is endometriosis and how does it impact your fertility? Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus. In addition to causing intense cramps and ongoing discomfort, it can lower your chances of becoming pregnant. Pelvic adhesions that form can block or damage the fallopian tubes and reduce your ovarian reserve, affecting the regular release of eggs. If you want to dive deeper into how this condition influences your fertility, read our simple guide to endometriosis and fertility. What are the early symptoms of endometriosis you should recognize? Detecting its signs early improves your reproductive prognosis. Although they vary, pay attention to: Menstrual pain so intense that it interferes with your daily activities. Changes in bowel movements (diarrhea or constipation) during your period. Discomfort or pain when urinating on your period days. Do not self-medicate: before taking any medication, consult a reproductive specialist if you want to increase your chances of pregnancy. How is endometriosis accurately diagnosed? The diagnosis combines a clinical exam, transvaginal ultrasound and, in some cases, laparoscopy. A specialized team will evaluate your history, pelvic pain and imaging findings. In this guide on endometriosis and fertility you will find more details on diagnostic techniques and next steps. What treatments exist to improve your quality of life and fertility? Depending on severity, your doctor might recommend: Hormonal therapy (oral contraceptives, progestins): reduces the growth of ectopic tissue. Laparoscopic surgery: removal of implants and adhesions. Assisted reproduction (IVF): if fertility is compromised, in vitro fertilization may be the most effective option. Remember that each body responds differently. A multidisciplinary approach ensures a personalized plan. Frequently Asked Questions 1. Does endometriosis always cause infertility? Not all women with endometriosis have trouble conceiving, but between 30% and 50% face reproductive challenges. The degree of impact depends on the extent of adhesions and your ovarian health. An early diagnosis and an appropriate treatment plan can greatly improve your chances of pregnancy. Trust assisted reproduction specialists to maximize your results. 2. Can I treat endometriosis if I want to get pregnant? Yes. Management includes minimally invasive surgical interventions and hormonal therapies that control pain and slow disease progression. After surgery, it’s recommended to plan for pregnancy quickly to take advantage of the optimal fertility window. If you have low ovarian reserve or tubal damage, in vitro fertilization (IVF) is a safe and effective alternative. 3. How long does it take for pain to improve after treatment? It depends on the treatment: some hormonal therapies reduce pain in 1–2 months, while relief after surgery can be noticed between 3–6 months. Ongoing follow-up helps adjust the therapeutic strategy. Combining pelvic physiotherapy and nutritional counseling also contributes to better pain management and improved quality of life. 4. What role does diet play in endometriosis? An anti-inflammatory diet—rich in omega-3 fatty acids, fruits, vegetables and fiber—can reduce pelvic inflammation and modulate pain. Avoid ultra-processed foods, excessive caffeine and saturated fats. Supplements such as vitamin D and probiotics have shown benefits. Consult your specialist to design a personalized nutritional plan. Sources Endometriosis. (2022). MedlinePlus. https://medlineplus.gov/ency/article/000915.htm Macer, M., & Taylor, H. S. (2012). Endometriosis and infertility: a review of pathogenesis and treatment. Obstetrics and Gynecology Clinics of North America, 39(4), 535–549. https://doi.org/10.1016/j.ogc.2012.08.009 Giudice, L. C. (2010). Clinical practice. Endometriosis. New England Journal of Medicine, 362(25), 2389–2398. https://doi.org/10.1056/NEJMcp1000274 Vercellini, P., Viganò, P., Somigliana, E., & Fedele, L. (2014). Endometriosis: pathogenesis and treatment. Nature Reviews Endocrinology, 10(5), 261–275. https://doi.org/10.1038/nrendo.2014.25 We know this journey can be challenging. You are not alone: seek support from an assisted reproduction specialist to answer your questions and guide you step by step toward your dream of becoming parents.

Starting an assisted reproduction treatment can be overwhelming: there will be ups and downs and moments of uncertainty. We know facing these challenges can make you feel alone. That’s why having the support of your partner, friends, or close family members is essential to keep you grounded and focused on the goal of having your baby. To dive deeper into this topic, see The Importance of Emotional Health in Fertility Treatment. What is emotional support in assisted reproduction and why is it key? Emotional support during assisted reproduction treatment includes understanding, empathy, and practical help from loved ones and professionals. Studies show that women who receive consistent accompaniment lower their cortisol levels (measured in μg/dL) and achieve higher pregnancy rates after IVF. This support reduces feelings of isolation and promotes healthier coping strategies. You can rely on your partner, friends, family, and specialized therapists at each stage: stimulation (hormone doses in IU), egg retrieval, embryo transfer, and the two-week wait. Their presence helps moderate anxiety spikes and improves your overall well-being, as explained in The Emotional Process of Men in Infertility, which highlights the male perspective and the importance of mutual support. How can your partner provide effective support? If you’re treated as a couple, your partner will be your main support. From day one, their participation in consultations, blood tests (e.g., 5 mL vials), and ultrasounds shares the emotional load. Attending stimulation appointments and joining you for the embryo transfer reinforces that team feeling. Open communication is key: ask what they need and share your feelings. Avoid assumptions: clarity in decisions—from choosing the protocol (for example, 150 IU of FSH per injection) to planning rest days—strengthens your commitment. Their unconditional support will give you the boost you need. Why is assessing both partners’ reproductive health so important? In 40% of couples with difficulty conceiving, male factors are involved. That’s why undergoing a simultaneous evaluation—semen analyses measuring volume (mL), concentration (million sperm/mL), and motility (%)—allows detection of issues like oligozoospermia. A joint diagnosis and a tailored treatment plan reduce uncertainty and foster teamwork: you face hormonal stimulation, egg retrieval, and embryo culture as a united couple. Strategies to improve communication with your partner It’s not always easy to express what you feel. Try these tips: Schedule regular times to talk about emotions and doubts. Allow space to process before discussing. Ask directly what support the other needs. Listen actively without immediately seeking solutions. Validate stress and allow vulnerability. Honest communication strengthens your bond and makes each challenge more manageable. Who else can be part of your support network? Your circle goes beyond your partner. Family and friends provide affection and understanding that reduce stress and promote relaxation, key benefits for fertility. According to MedlinePlus, high stress can affect ovulation and sperm quality. Sharing your experience with trusted people breaks taboos—infertility affects 1 in 6 couples—and brings concrete help, from preparing healthy meals to accompanying you to appointments. How do others’ experiences contribute to the process? Connecting with those who have been through the same thing normalizes your feelings and reminds you that infertility isn’t your fault. Success stories and coping strategies offer hope and inspiration. Support groups—in-person or online—are safe spaces to share fears, celebrate achievements, and discover resources that strengthen your resilience. What does Ingenes’s Emotional Support Service (SEI) include? If you’re undergoing assisted reproduction at Ingenes, we offer the Emotional Support Service (SEI) as part of your treatment. In guided sessions, patient groups share experiences under the supervision of specialized therapists who provide tools to improve your emotional well-being. Your decision to become a mother or father is powerful. You don’t have to face this journey alone: your partner, family, friends, and the entire Ingenes team will be your anchor until you have your baby in your arms. Frequently Asked Questions How does stress affect assisted reproduction success? High stress can disrupt hormone production, hinder ovulation, and reduce semen quality. Studies show that relaxation techniques and psychological support lower cortisol levels (μg/dL) and improve embryo implantation rates. Incorporating therapies like mindfulness or yoga and having a support group creates a calmer environment, optimizing the chances of pregnancy. What role does the partner play in ovarian stimulation? Your partner’s presence at each appointment strengthens your bond and reduces anxiety. Attending visits together, reviewing follicles on ultrasound (measured in mm), and deciding on the medication plan (for example, 150 IU of FSH) facilitates decision-making. Their unconditional support fosters teamwork, boosts morale, and promotes treatment adherence. Why is joining a support group important? Being part of communities with other women and men undergoing similar treatments allows you to exchange experiences, coping strategies, and practical recommendations. This reduces isolation and provides motivation throughout the process. Facilitators, typically specialized psychologists, guide sessions to address emotional topics, improve communication, and share success stories. When should I seek additional professional help? If you experience intense anxiety, depressive episodes, or feelings of hopelessness that interfere with your daily life, it’s essential to see a psychologist or psychiatrist experienced in reproductive health. Avoid self-medicating without supervision. A reproductive specialist will advise you on safe medication and complementary therapies to optimize your physical and emotional well-being. References American Society for Reproductive Medicine. (2020). Stress and Reproduction. https://www.asrm.org MedlinePlus. (2021). Fertility and Stress. U.S. National Library of Medicine. https://medlineplus.gov World Health Organization. (2010). WHO laboratory manual for the examination and processing of human semen (5th ed.). doi:10.1007/978-3-642-02240-2 Li, S., Huang, T., Zheng, Y., Muka, T., & Hu, F. B. (2019). Stress and semen quality: a systematic review and meta-analysis. Human Reproduction Update, 25(3), 340–364. doi:10.1093/humupd/dmz006 Remember that your emotional well-being is as important as your physical health. Don’t hesitate to seek support and always consult a fertility specialist for proper guidance.

El clomifeno es un medicamento que promueve la ovulación, y puede incrementar las probabilidades de un embarazo si es administrado de forma adecuada por médicos especialistas. Te explicamos cómo aquí.
Una reserva ovárica baja puede comprometer tus probabilidades de tener un bebé. Te decimos cómo conocer la tuya y tus opciones para ser mamá.

In the world of fertility treatments, advancements are constantly being made to help prospective parents realize their dreams. In this article, we will explore the promising field of endometrial regeneration, an innovative approach with the potential to improve pregnancy success rates and support fertility treatments. Understanding Endometrial Regeneration The endometrium, the delicate inner lining of the uterus, plays a vital role in the success of pregnancy. It provides a suitable environment for the embryo to implant and develop. However, in some cases, the endometrium may be thin or damaged, reducing the chances of successful implantation. This is where the concept of endometrial regeneration comes into play: an innovative treatment designed to improve the conditions of the uterine lining and achieve pregnancy. The Power of Regenerative Medicine Regenerative medicine is an exciting scientific field that can be of great interest to women pursuing the dream of motherhood. It focuses on helping to restore damaged tissues and organs. In the case of endometrial regeneration, the aim is to stimulate the growth and repair of the uterine lining. If you have ever experienced issues with your uterine lining, such as thinning or damage from previous miscarriages, this innovative technique could be an option to improve your chances of getting pregnant and having a successful pregnancy. Endometrial regeneration opens new hopes and opportunities in the field of fertility, providing a promising option to fulfill your dream of starting a family. Increasing Pregnancy Success Rates One of the highlights of endometrial regeneration is its potential to increase your chances of getting pregnant. By creating an optimal environment within your uterus, this innovative approach improves the chances of successful embryo implantation and development. This can make a difference for you and thousands of women seeking motherhood, offering a hopeful option. Personalized Care for Optimal Results We strongly believe in providing you with personalized care that suits your unique needs. This customized care approach also applies to the options offered by regenerative medicine. It is important to choose a dedicated team of experts who will work closely with you, thoroughly evaluating your specific circumstances and developing a personalized treatment plan. Through a combination of advanced techniques and compassionate support, our goal is to help you maximize your chances of achieving a successful pregnancy. One Step Closer to Motherhood Endometrial regeneration represents a significant advancement in the field of fertility treatments, bringing renewed hope and potential to those longing to become parents. While this field is still evolving, promising research and clinical trials continue to shed light on its effectiveness. Remember that you are never alone. At Ingenes, we are here to accompany you every step of the way, providing unwavering support, expert guidance, and the commitment to make your dreams come true.

Las mujeres con ovario poliquístico pueden tener hijos. Claudia te cuenta cómo ella lo logró después de buscar a su bebé por más de 5 años.

Berenice tuvo abortos recurrentes debido a que vive con ovario poliquístico. Conoce su historia y cómo logró a su bebé en su 3er. ciclo de FIV.

Aneuploidía es una alteración genética que puede presentarse en el embrión y comprometer su desarrollo. Te decimos cuáles son sus principales causas y cómo prevenirla.

Baja reserva ovárica y FIV positiva en su tercer intento, conoce a Claudia, quien se convirtió en mamá después de varios tratamientos fallidos.

Fernanda tuvo su embarazo con ovario poliquístico, al realizar un tratamiento multiciclo de Fertilización In Vitro, aquí te cuenta su historia.

Soy Claudia, tengo endometriosis y quedé embarazada. Conoce su historia y cómo vive este padecimiento que afecta a 7 millones de mexicanas.
Te has preguntando: ¿Con ovario poliquístico puedo quedar embarazada? Karina lo hizo, conoce su historia y cómo tuvo a su pequeña Romina.

Leslie tenía endometriosis y pasó varios intentos de embarazo con FIV, para lograr a su pequeña Martina en su último ciclo de 4 fertilizaciones.

El estrés por quedar embarazada no debe menospreciarse. Conoce a Elba y cómo logró a su bebé atendiendo su salud reproductiva y emocional.

Con un tratamiento de Reproducción Asistida multiciclo, Marisol y su esposo lograron tener a sus cuatitos en su tercer ciclo de Fertilización In Vitro.

Mira estos consejos para mejorar la fertilidad y tener más posibilidades de ser mamá. Recuerda que no estás sola en esto, estamos para ayudarte.