Don't miss our updates



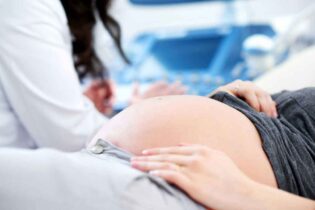
Diabetes mellitus is characterized by high blood glucose levels and, if left uncontrolled, can affect a man’s fertility in several ways. The first step in controlling diabetes is to eat a healthy diet and exercise regularly. If this is not enough, you may need to take medication or insulin injections. Diabetes treatment is usually enough to restore fertility. Otherwise, in vitro fertilization with intracytoplasmic sperm injection (IVF+ICSI) is the treatment of choice to achieve pregnancy. It is advisable to perform a sperm DNA fragmentation test before starting any assisted reproduction treatment since diabetes mellitus damages sperm DNA and a high fragmentation rate could affect the success rates of these procedures. What is diabetes mellitus? Diabetes mellitus is a disease in which the body does not produce enough insulin or does not use it properly. Insulin is a hormone that transforms sugar, starch, and other foods into the energy we need daily. According to data from the World Health Organization, diabetes mellitus affects 200 million people worldwide, and it is estimated that by 2030 there will be 366 million diabetics. Diabetes mellitus is characterized by high levels of glucose in the blood and if not controlled can affect a man’s fertility in several ways: Women with uncontrolled diabetes may have ovulation problems or be more prone to cervical-vaginal infections. Similarly, high blood sugar levels increase the risk of miscarriage and can cause birth defects in the fetus or even lead to excessive growth (macrosomia) and complications during delivery. The main symptoms of diabetes mellitus The main symptoms of diabetes mellitus are: If you have any of these symptoms you should consult a doctor immediately, as timely treatment of diabetes can prevent various health problems. Causes of diabetes mellitus Diabetes mellitus occurs because the body does not produce enough insulin or does not use it properly. Some factors that increase the likelihood of developing diabetes include: It is important to note that diabetes can be hereditary and men with parents or brothers who suffer from it are more likely to develop it. How is diabetes mellitus diagnosed? In addition to a physical examination and a review of the patient’s medical history, a fasting blood glucose test is necessary. A person with a blood glucose level of 126 mg/dl or higher has diabetes and should be treated. People with diabetes mellitus need to have regular tests to make sure their glucose levels are under control. If you have had trouble conceiving and are overweight or if someone in your family has diabetes, it is recommended that you have a blood test to rule out this disease. Treatments for achieving pregnancy when you have diabetes mellitus The first step to controlling diabetes is to eat a healthy diet and exercise regularly. If this is not enough to keep your blood sugar levels under control, you may need to take medications such as sulfonylureas and metformin or take insulin injections. Diabetes treatment is usually enough to restore fertility. Diabetics under good medical control, with good body weight and normal blood glucose and cholesterol levels, usually have better quality semen and ejaculate normally. Otherwise, in vitro fertilization with intracytoplasmic sperm injection (IVF+ICSI) is the treatment of choice to achieve pregnancy because it makes it possible to inject a single sperm directly into the cytoplasm of a mature egg using a microscopic needle. It is advisable to perform a sperm DNA fragmentation test before starting any assisted reproduction treatment since a high fragmentation rate could affect the success rates of these procedures. In the case of a man suffering from anejaculation or if there are no good quality sperm in the ejaculate, it is possible to recover them using epididymal aspiration or testicular biopsy. Patients with erectile dysfunction can take medication to restore erections. It is important to note that in cases of retrograde ejaculation, it is possible to recover sperm directly from urine to use in assisted reproduction treatments after a washing process.

When we talk about fertility treatments, we often think of the medical and scientific solutions that allow couples and single individuals to fulfill their dream of having a baby. But we understand that the journey also has a very strong emotional component. At Ingenes we know that taking care of your emotional health is essential for the treatment to work, which is why we offer specialized services to support you at every stage. What is emotional health and why is it key in fertility? Emotional health is the balance that helps us manage stress, anxiety, and doubts that arise during the reproductive process. With hormones, procedures, and constant appointments, it’s normal to experience ups and downs. Staying balanced not only improves your well-being but can also enhance hormone production and uterine receptivity. Do not self-medicate without consulting your doctor. If you want to increase your chances of pregnancy, always see a specialist in Assisted Reproduction. Emotional support services at Ingenes Our comprehensive program complements your treatment with: Individual and couple therapy: 50–60 minute sessions with psychologists expert in assisted reproduction to manage stress. Support groups: Weekly meetings to share experiences and feel accompanied. Workshops and talks: 90-minute activities on coping techniques, menstrual cycle, and emotional preparation. Mindfulness and relaxation: Breathing exercises, guided meditation, and adapted yoga, with daily practices of 15–20 minutes. Impact of emotional support on outcomes Chronic stress raises cortisol and disrupts the hypothalamic-pituitary axis, affecting ovulation and sperm quality. Having emotional support in assisted reproduction reduces these effects and creates a more favorable environment for implantation. Moreover, emotional backing strengthens your motivation and commitment to the treatment, improving coordination with your medical team and optimizing ovarian stimulation protocols. Additional benefits of emotional care Less anxiety: Techniques to calm heart rate and relax muscles. Better physical health: A positive emotional state improves sleep and recovery. Stronger relationship: Open communication and conflict resolution. Greater resilience: Facing setbacks with hope and a proactive attitude. Complement your well-being with the importance of nutrition in fertility treatment, where you’ll find dietary guides that support your hormonal and emotional balance. Frequently Asked Questions Can anxiety reduce my chances of pregnancy? Yes. High cortisol interferes with gonadotropin production, which is essential for ovulation and spermatogenesis. Practicing diaphragmatic breathing for 10 minutes a day helps normalize levels. Also, sleeping 7–8 hours daily is crucial for recovery and immune function. How do I choose the right therapist? Choose psychologists certified in perinatal psychology or reproductive mental health with experience in IVF or ICSI. Look for reviews from other patients and a trial session to ensure you feel comfortable and supported. When should I join a support group? From the start of your treatment you can benefit from sharing experiences. If you feel emotional fatigue, persistent sadness, or guilt, joining a group will help you express your fears and receive support. Online or in-person support? Online support offers flexibility, but in-person therapy facilitates emotional connection. Combining both formats enhances results. If you’re far from a center, schedule regular virtual sessions and at least one in-person consultation at the beginning. Sources Consulted American Society for Reproductive Medicine. (2022). Stress and Reproductive Health. Fertility and Sterility. MedlinePlus. (2023). Anxiety Disorders. U.S. National Library of Medicine. World Health Organization. (2023). Mental Health in Reproductive Care. WHO Fact Sheets. National Institutes of Health. (2021). Mindfulness-Based Interventions for Stress Reduction in Infertility. Journal of Psychosomatic Obstetrics & Gynecology. Remember: you are not alone on this journey. Taking care of your emotional health is as important as medical treatment. If you need it, see a fertility specialist for the comprehensive care you deserve. We are with you!

On September 4 we celebrate World Sexual Health Day, promoted by the World Association for Sexual Health. It’s a time to talk about sexuality without taboos, with clear information and recognizing that it’s an essential part of our health and well-being. At Ingenes Fertility Institute in Mexico, this date reminds us that sexual health includes fertility, reproductive rights, and informed decisions. Every story deserves judgment-free support. What is sexual health and why does it matter? According to the WHO, sexual health is a state of physical, emotional, mental, and social well-being in relation to sexuality, not merely the absence of disease. It involves being able to enjoy safe and pleasurable experiences free from coercion and discrimination. Talking about sexual health goes beyond intimate relationships. It includes: Knowing your own body. Making informed reproductive decisions. Access to quality medical care. Respect for sexual and gender diversity. Prevention and treatment of STIs. Family planning and fertility. This comprehensive approach links sexual and reproductive health as two sides of the same coin. How is fertility related to sexual well-being? In many cultures we only talk about avoiding unwanted pregnancies or STIs. But when you face difficulties conceiving, fertility becomes a crucial part of your sexual health. At Ingenes we have spent over 20 years supporting thousands of women, men, and couples who didn’t know they could seek specialized help or felt it was a taboo topic. Celebrating World Fertility Day shows that questions like “Why can’t I get pregnant?” are valid and necessary. What medical factors affect fertility? Some conditions can make conception difficult without showing clear symptoms: Hormonal imbalances Low ovarian reserve Endometriosis Polycystic ovary syndrome (PCOS) Blocked fallopian tubes Male factor (low sperm concentration or motility) Reproductive immunology Genetic factors Many variations are confused with normal cycles, so a comprehensive evaluation including gynecology, endocrinology, and reproductive immunology is essential. How does emotional health support fertility? Failed attempts can cause stress, anxiety, and relationship tensions. Emotional well-being is as fundamental as medical treatment. At Ingenes we include psychological support from the start. Our specialists help you manage emotions, strengthen resilience, and maintain hope. Lifestyle habits that protect your fertility Some recommendations: Under 35: evaluation after 12 months of trying. Over 35: after 6 months. If you plan to delay pregnancy, consider an ovarian reserve study. Manage chronic conditions (diabetes, hypertension, thyroid). Do not self-medicate without consulting a doctor. Maintain a balanced diet, exercise regularly, and manage stress. Information and professional guidance strengthen your sexual and reproductive health. Who can access assisted reproduction? We serve diverse families: single women, same-sex couples, trans people, and anyone who wants to become a mom or dad. We offer egg, sperm, or embryo donation and the ROPA method for shared motherhood. We also celebrate International Men’s Health Week, because male fertility is part of this inclusive vision. Immediate steps to care for your fertility Schedule your annual gynecological exam. Talk with your partner about family planning. If you’ve had difficulties, get a fertility evaluation. Share scientific and empathetic information with your circle. Don’t ignore severe menstrual pain, irregular bleeding, or hormonal changes. Seek psychological support if emotions overwhelm you. Before using any medication, consult a specialist in assisted reproduction. Full sexuality includes your right to become a mom or dad At Ingenes we believe sexual health encompasses the desire to have a child if you choose. We combine science, empathy, and real results to make your family dream possible. Talking about sexuality is also talking about hope, family, and the future. Frequently Asked Questions 1. What should I do if I’ve been trying to conceive for a while? Keep a record of your cycles and ovulation signs for at least three months. Under 35, seek help after one year of trying; over 35, after six months. The evaluation includes hormone levels (FSH, AMH in ng/mL) and an ovarian reserve ultrasound. A reproductive endocrinologist will interpret results and suggest lifestyle adjustments, treatments, or assisted techniques. 2. How does stress affect fertility? Chronic stress alters key hormones like cortisol, estrogen, and progesterone, making ovulation and sperm quality more difficult. It can reduce sexual desire and create relationship tensions. At Ingenes we use cognitive-behavioral therapy, mindfulness, and stress management so you can face this process better and strengthen your support network. 3. Can I preserve my fertility if I’m not ready for pregnancy? Yes. Egg vitrification is ideal for postponing motherhood. After controlled ovarian stimulation guided by ultrasound and tests, eggs are retrieved under sedation and stored at –196 °C in liquid nitrogen. It’s best done before age 35. 4. What role does male fertility play and how is it evaluated? The male factor accounts for up to 50 % of infertility cases. A semen analysis measures volume (mL), concentration (million/mL), motility (%), and morphology (% normal). Hormones (testosterone, FSH) are also evaluated and, if needed, genetic studies. Improving male fertility includes a balanced diet, exercise, avoiding tobacco, excessive alcohol, and localized heat. If abnormalities are found, the specialist may recommend medical treatments, varicocele surgery, or ICSI. References World Health Organization. (2015). WHO guidelines on prevention and treatment of maternal peripartum infections. https://doi.org/10.1017/9781108166592 American Society for Reproductive Medicine. (2020). Definitions of infertility and recurrent pregnancy loss. Fertility and Sterility, 113(6), 1252–1253. https://doi.org/10.1016/j.fertnstert.2020.03.021 MedlinePlus. (2023). Infertility. U.S. National Library of Medicine. https://medlineplus.gov/infertility.html Practice Committee of the American Society for Reproductive Medicine. (2018). Emotional aspects of infertility. Fertility and Sterility, 110(4), 611–619. https://doi.org/10.1016/j.fertnstert.2018.06.007 We know this journey can be challenging. If you have questions or need guidance, consult a specialist in assisted reproduction. We’re with you every step of the way.

At Ingenes we know that each journey to motherhood or fatherhood is unique. We are proud to share an award that reflects the effort and passion of our team in Guadalajara. What does this international recognition mean and why does it matter to you? Recently, Ingenes – Guadalajara received a certificate of participation from the Latin American Registry of Assisted Reproduction (RLA) and ICMART. This speaks to our transparency and commitment to high global standards. For you, it means receiving care backed by data and compared with the best clinics in Latin America and the world. How does Ingenes Guadalajara contribute to the RLA registry? In 2022, Ingenes – Guadalajara reported data on IVF cycles, follicular fluid volume, and number of viable blastocysts transferred. With hundreds of data points—for example, implantation rates per 100 transfers—we help the RLA improve efficiency and safety across Latin America. What do you gain from our participation in global registries? By sharing data with RLA and ICMART, we refine stimulation protocols, adjust gonadotropin dosages, and optimize embryo culture. All to increase your chances of success and protect your health, avoiding risks like ovarian hyperstimulation syndrome. Medical Team of Ingenes Guadalajara Advanced services: surrogacy and cross-border care In addition to IVF, we offer surrogacy in Mexico with legal advice and full clinical protocols. And if you wish, we coordinate your treatment between Mexico and the U.S. so you can take advantage of our laboratories and maintain continuity of care. Every day our team in Guadalajara works with heart and the best technology to support you in this dream of becoming a family. This recognition motivates us to keep learning and sharing achievements with all of you. Ingenes – Committed to your dream of becoming a family. Frequently Asked Questions 1. What is the Latin American Registry of Assisted Reproduction (RLA) and how does it impact my treatment? The RLA collects information from clinics like ours: oocyte yield, fertilization rates per ten oocytes, and pregnancies per transfer. With this data, we improve our protocols to offer you safer and more effective treatments. Transparency of results gives you confidence, and clinical decisions are based on real evidence. 2. How do I know if surrogacy in Mexico is right for me? Surrogacy in Mexico follows state laws. At Ingenes we guide you through eligibility criteria, legal contracts, and medical protocols (endometrial preparation, embryo transfers). Our multidisciplinary team supports you from psychological evaluations to neonatal care. 3. What are the IVF success rates at Ingenes Guadalajara? Our implantation rates exceed 40% per blastocyst transfer, and the live birth rate is over 50% for women under 35. These numbers come from our RLA reports, with standardized laboratory conditions (37 °C incubators, controlled CO₂ levels). 4. Can I start my treatment in Mexico and finish it in the U.S.? Yes. You can do your ovarian stimulation and egg retrieval in Mexico with recombinant FSH, vitrify your embryos, and send them to the U.S. Our logistics team handles the entire cryotransfer and customs documentation process. Sources Consulted International Committee for Monitoring Assisted Reproductive Technologies. (2023). ICMART Annual Report. Retrieved from https://doi.org/10.1000/icmart2023 Latin American Registry of Assisted Reproduction. (2022). RLA Data Summary. Retrieved from https://doi.org/10.1000/rla2022 MedlinePlus. (2024). Assisted Reproductive Technology. Retrieved from https://medlineplus.gov/assistedreproductive.html Practice Committee of the American Society for Reproductive Medicine. (2023). Guidelines on Ovarian Stimulation. Fertility and Sterility, 119(4), 823–829. Retrieved from https://doi.org/10.1016/j.fertnstert.2023.01.045 We know how important this journey is for you. If you have questions or want to start your treatment, consult a specialist in assisted fertilization: we are here to support you every step of the way.

When it comes to addressing infertility and the desire to become parents, low-complexity treatments are often the recommended starting point for many couples. This type of treatment is particularly relevant for those who are facing difficulties in conception but have not yet explored medical options. In many cases, couples are not aware of their infertility situation until they encounter obstacles to conceiving naturally. It is recommended that if a couple has been trying to have a baby for a year without success, and the woman is under 35 years old, they should consider consulting with an assisted reproduction specialist. An assisted reproduction specialist not only provides an accurate diagnosis but can also recommend the most effective treatment for the couple’s specific needs. Infertility can be the result of a variety of factors, and only a professional evaluation can determine the most appropriate path forward. At Ingenes Fertility Institute in Mexico, we often suggest low-complexity treatments for couples with women under 35 years of age. This is because the quality and quantity of eggs are generally more favorable in younger women. The quality of the egg is a crucial factor since it directly influences the ability to form healthy embryos, with an adequate number of chromosomes and the energy necessary to develop successfully after fertilization. It should be noted that, although these treatments may be more accessible from a financial point of view, they do not offer a guarantee of success. The effectiveness of these treatments may be limited compared to more comprehensive options. For this reason, an evaluation by an assisted reproduction specialist is essential. At Ingenes Fertility Institute in Mexico, the specialist can recommend the Comprehensive BEC Programs, designed to maximize your chances of bringing your baby home. Low Complexity Treatments in Assisted Reproduction Below, we detail the main low-complexity techniques and how they can be the first step toward realizing your dream of having a baby. – Ovulation Induction: This treatment is ideal for women under 32 years of age who have ovulation problems, such as polycystic ovary syndrome or anovulation. Through the use of medications, the ovaries are stimulated to regulate the menstrual cycle and increase the chances of ovulation and, therefore, conception. – Scheduled Intercourse: This technique involves detailed monitoring of the woman’s ovulatory cycle. The optimal time for sexual relations is determined, thus significantly increasing the chances of pregnancy. It is a less invasive option and can be particularly effective for couples without severe fertility problems. – Artificial insemination: Artificial insemination consists of placing previously prepared and selected sperm directly into the woman’s uterus during her ovulation period. This technique improves the fertility potential of sperm through a process called sperm capacitation. This process includes washing and centrifugation techniques that purify the sample, eliminating impurities and selecting the highest quality and most motile sperm. – Sperm Training: An essential step in artificial insemination, sperm capacitation improves the chances that selected sperm will fertilize the egg. This laboratory procedure is crucial to ensure that only the fittest sperm are used in the treatment. At Ingenes Fertility Institute in Mexico, we understand the importance of each step on your path to parenthood. From your first consultation, we provide you with an accurate diagnosis and guide you through the most appropriate treatment options for your case. Our goal is to give you the best possible opportunity to fulfill your dream of having a baby. Don’t hesitate to reach out to us for more information and start your journey toward finding your baby.

Michelle Obama’s brave revelation about her experience with pregnancy loss has touched the hearts of millions of women around the world. Her story is not only one of pain and loss but also one of resilience and hope. By openly sharing her journey through infertility, Michelle has shed light on a topic that often remains in the shadows, surrounded by stigma and silence. At Ingenes, we recognize the importance of these personal narratives and how they can inspire and encourage other women facing similar challenges in their desire to start a family. Michelle’s tragic experience highlights an issue that affects a surprisingly large number of couples around the world. Pregnancy loss, a deeply moving and life-changing event, can leave lasting emotional scars and unanswered questions. At Ingenes, we are committed to providing a safe and supportive space where these stories can be shared and where couples can find a sense of community and understanding. Our mission at Ingenes goes beyond offering cutting-edge fertility treatments. We strive to understand the emotional and physical complexities our patients face on their path to parenthood. Michelle Obama’s story not only motivates us to continue our work, but also reminds us of the importance of approaching these issues with sensitivity, care, and a deep respect for each person’s individual experiences. What lessons can we learn from Michelle Obama’s pregnancy loss? In “Becoming”, Michelle Obama shares the intimate details of her experience with miscarriage. This honest account reminds us that pregnancy loss affects 10–20% of known pregnancies and is often underreported due to stigma. By speaking openly, she has given voice to many women who feel alone in their grief and inspired them to seek support. How does In Vitro Fertilization work and when should it be considered? After their loss, the Obamas opted for In Vitro Fertilization (IVF). IVF involves retrieving mature eggs and sperm, combining them in a lab dish, and transferring viable embryos into the uterus. Success rates vary by age and clinic but can range from 30% to 50% per cycle. At Ingenes, we tailor protocols—dosing hormones in IU and monitoring follicle growth in mm—to optimize outcomes. Why is emotional support crucial during infertility treatments? Pregnancy loss and fertility treatments carry a heavy emotional toll. At Ingenes, we complement our medical protocols with counseling services, support groups, and mind–body therapies. Studies show that women who receive psychosocial support have higher treatment adherence and report reduced anxiety and depression. Our approach is rooted in empathy: we listen, validate your feelings, and accompany you at every step. How can personalized treatment plans improve fertility outcomes? Couples respond differently to medications and protocols. By analyzing AMH levels in ng/mL, antral follicle counts, and genetic factors, our team crafts individualized plans. Whether it’s adjusting the gonadotropin dose from 150 IU to 300 IU or selecting time-lapse embryo monitoring, personalization boosts implantation rates. Michelle Obama’s story is a source of inspiration and hope. At Ingenes, we strive to provide our patients with the best fertility care and treatments, helping them turn their dreams of becoming mothers into reality. For more success stories, explore Celebrities and In Vitro Fertilization: Stories of Success and Hope. Avoid self-medicating without consulting a doctor. Before resorting to this medication, you need to see a specialist in assisted reproduction, particularly if you are looking to increase your chances of getting pregnant. Frequently Asked Questions What are the most common causes of pregnancy loss? Chromosomal abnormalities in the embryo account for nearly 50% of miscarriages, especially in the first trimester. Other factors include uterine malformations, hormonal imbalances like low progesterone, thyroid disorders, or uncontrolled diabetes. Lifestyle factors—smoking, excessive caffeine, or obesity—can also increase the risk. How long should I wait after a miscarriage before trying again? Medical guidelines suggest waiting at least one to three regular menstrual cycles before attempting conception to allow the endometrium to recover and ensure accurate dating of a new pregnancy. Emotional readiness is equally important—seek counseling if feelings of grief or anxiety persist. When is it appropriate to consider assisted reproduction? Couples under 35 who have tried unprotected intercourse for 12 months without success, or women over 35 who have tried for six months, should be evaluated for infertility. Factors like low ovarian reserve (AMH
To understand how hypothyroidism influences fertility, first you need to know that the thyroid gland produces two key metabolic hormones: T4 (thyroxine) and T3 (triiodothyronine). This butterfly-shaped gland is located at the front of the neck, just below the Adam’s apple. Although there are many thyroid conditions, in this article we will focus on hypothyroidism and its impact on female fertility. Thyroid gland in the human body What is hypothyroidism and how does it affect fertility? Hypothyroidism occurs when the thyroid does not produce enough T3 and T4. In women it can disrupt ovulation, cause irregular menstrual cycles, and complicate conception. Do not self-medicate: before taking any medication, consult a Reproductive Medicine specialist. They will evaluate your case and increase your chances of pregnancy. Key symptoms in women trying to conceive Extreme fatigue Unexplained weight gain Cold intolerance Dry skin and brittle hair Irregular or absent menstrual cycles Mild depression or persistent constipation If you notice any of these changes, share them with your doctor. Recurrent miscarriages or difficulty conceiving can be warning signs. Most common causes of hypothyroidism Autoimmune thyroiditis (Hashimoto’s) Radiation therapy to the head or neck Thyroid surgery Iodine deficiency Medications (lithium, amiodarone) Pituitary disorders affecting TSH In many cases the cause is not identified, so early diagnosis is vital. Diagnosis before trying to conceive The endocrinologist will measure your neck, skin, weight, and heart rate. Then they will order a blood test to measure TSH. A value above 3.5 mU/L suggests hypothyroidism. Free T3 and T4 may also be measured to assess severity. With this data, your doctor will design a treatment plan to protect your health and that of your future baby. Treatment options if you plan to have a baby The standard treatment is levothyroxine, adjusted according to your weight (approx. 1.6 μg/kg per day) and lab results. Every body is unique: consult a Reproductive Medicine specialist to determine your dose and monitor your hormone levels. For more information, check our article Hypothyroidism and Fertility or explore Hyperthyroidism and Fertility. Ingenes family who overcame thyroid issues Frequently asked questions 1. Does hypothyroidism cause irreversible infertility? With treatment and TSH control, most patients regain ovarian function and can conceive naturally or with assisted reproduction techniques. 2. How do TSH levels influence embryonic development? TSH regulates T3 and T4, essential for ovarian follicle maturation and a receptive endometrium. Keeping TSH between 0.5–3.5 mU/L improves implantation and reduces miscarriage risk. 3. Can I improve my thyroid with diet? Include iodine (fish, seaweed, dairy), selenium (nuts), and zinc (lean meats). Avoid excessive raw goitrogenic foods like soy and broccoli. Always consult your nutritionist or endocrinologist before changing your diet. 4. Is levothyroxine treatment safe during pregnancy? Yes. Levothyroxine is the treatment of choice: it does not actively cross the placenta and ensures adequate hormone levels. During pregnancy, your dose may be adjusted; monitor TSH every 4–6 weeks. Sources Consulted American Thyroid Association. (2017). Guidelines for diagnosis and management of hypothyroidism. Thyroid, 27(3), 315-389. MedlinePlus. (2022). Hypothyroidism. https://medlineplus.gov/hypothyroidism.html de Groot et al. (2012). Management of thyroid dysfunction during pregnancy. J Clin Endocrinol Metab, 97(8), 2543-2565. Stagnaro-Green et al. (2011). Clinical practice guideline: thyroid disease in pregnancy. Thyroid, 21(10), 1081-1125. Remember that every case is unique. We are with you on this journey and encourage you to consult a fertility specialist for the personalized guidance you deserve.

At Ingenes we understand that every journey to motherhood or fatherhood is unique. Here we outline the main fertility treatments, how they work and how our cutting-edge technology and personalized protocols support you every step of the way. Artificial insemination: what it is and when to consider it Artificial insemination places washed sperm (0.5–1 mL) directly into the uterus near ovulation. It’s ideal if your partner has mild male infertility, no specific cause is found or there’s an issue with cervical mucus. At Ingenes we personalize hormonal stimulation and the timing of the procedure according to your cycle, increasing success rates without resorting to more invasive treatments. Never self-medicate: always consult a specialist. In Vitro Fertilization (IVF): What it involves and who benefits IVF combines eggs and sperm in the laboratory. After ovarian stimulation with 150–300 IU of gonadotropins daily, we retrieve mature oocytes, fertilize them in a culture medium and transfer the highest-quality embryo (8–10 cells on day 3 or blastocyst on day 5) into the uterus. It’s recommended for tubal factor, endometriosis, severe male infertility or if insemination has failed. Before starting, consult a Reproductive Medicine specialist. Prior recommendations: maintain your physical and emotional health. We help you prepare holistically. ICSI: When microinjection is the best solution ICSI injects a single sperm directly into the egg, ideal for severe oligozoospermia, azoospermia, low motility or previous fertilization failures. Our embryologists use high-precision micromanipulators to ensure each oocyte receives a viable sperm, overcoming male infertility barriers. Egg or Sperm Donation: When to consider it If gamete quality is suboptimal, a donor may be the solution. Candidates undergo genetic, infectious and psychological screening; we match donors by physical characteristics and medical history. We can use fresh or frozen embryos and our success rates exceed 60% per transfer. All under strict confidentiality and constant support. At Ingenes we combine experience and advanced technology to support you from the first consultation through embryo transfer and beyond. Our team provides attentive, dedicated care. Visit Your Journey to Motherhood to learn more and take the next step on your path to parenthood. Frequently Asked Questions What should I do before starting fertility treatments? Schedule a comprehensive evaluation: hormonal profile (FSH, LH, AMH) and pelvic ultrasound. Achieving a BMI of 18.5–24.9, quitting smoking and taking 400 µg of folic acid daily optimizes receptivity. Avoid self-medication and always consult your specialist. How do I know if I need ICSI instead of IVF? ICSI is recommended when concentration is under 5 million/mL, motility drops below 32% or after failed IVF cycles. Advanced semen analyses and genetic tests guide this decision along with your reproductive history. Can I use donor gametes if I have a genetic condition? Yes. If you carry hereditary mutations (BRCA1/2, cystic fibrosis), using a donor reduces risks. We conduct exhaustive genetic screening on donors and offer genetic counseling to help you make the best choice. What are the effects of ovarian stimulation? Common effects include bloating and mood changes. Rarely (1–2%) ovarian hyperstimulation syndrome may occur: abdominal pain, nausea and fluid retention. We monitor estradiol levels and follicles by ultrasound to adjust doses and prevent complications. Sources American Society for Reproductive Medicine. Committee Opinion No. 814. Fertility and Sterility, 118(2), 484–495 (2022). Practice Committee ASRM. Diagnostic Evaluation of the Infertile Female. Fertility and Sterility, 116(3), 673–684 (2021). MedlinePlus. Intrauterine insemination (2023). MedlinePlus. In vitro fertilization (2023). We are with you at every step. If you have doubts or need personalized guidance, consult a Reproductive Medicine specialist to guide and support you on this hopeful journey.